I really like my cardiologist. She called me again today in response to a message I sent her late last week. Instead of writing a reply, she decided to call instead. I had asked her about the “aggressive” dialysis comment from the UCLA transplant cardiologist and she said the echocardiogram showed I still have fluid in my lungs. She recommended that I stop taking my hypertension medication before dialysis so there is more “room” for the blood pressure to drop as the machine removes excess fluid. I told her that the dialysis center was already removing more fluid, and last two sessions showed a drop in blood pressure instead of the typical increase. Anyways, she ordered another echocardiogram to be done in about two week. Hopefully I will be rid of the pulmonary edema and UCLA will be satisfied with the health of my heart.
Author: mybadkidney
“Final” Podiatrist Appointment
I went to see my podiatrist again today. He wanted to check out my toe after he took out the stitches three weeks ago. It bled more for a few days but the wound is completely dry now. The podiatrist said to come back in six months and don’t step on anything sharp again. Thanks!
He also gave me a referral to get orthopedic shoes. The last time I went, which was several years ago, they showed me a bunch of ugly-assed shoes. I ended up choosing a New Balance MX624 cross-trainer. I remember being charged over $200 for the pair, which was paid by insurance. Since then, I’ve been buying the same shoes on Amazon for ~$70. Today, as my podiatrist was writing the referral, he said that Medicare should pay for the shoes. I guess that is the problem with the healthcare industry. Most people have insurance, either Medicare or private insurance through work. Because we don’t see or pay the entire bill, we don’t shop for the best deals. When was the last time you saw a price list at your doctor’s office or in a hospital? Never, right? I have no incentive to price shop even though my taxes pay for Medicare, and my company pays for other insurance claims. Since I’m also a shareholder of my company, I’m indirectly paying the claims.

One-Year Post-Surgery
It’s been a year since my open heart bypass surgery. The surgery was on November 14, 2019. I think they started at around noon and I woke up at 1:30 am the next day. I was on the operating table for about seven hours and it took another five to wake up. I was technically “dead” during the surgery since they had to stop my heart and lungs to operate but I don’t remember anything. One moment I was getting wheeled into the OR, and the next moment I was trying to wake up.
I guess you can call it a second birthday since I would probably be dead now if I didn’t have the surgery. From the ER lab results and subsequent stress test and CAT scan, I probably had a heart attack days or weeks prior to the surgery, and would like had more if they didn’t replace my clogged arteries. However, it has been a difficult year, made much worse by COVID-19. I had my diabetes under control for a few years but being on dialyis and being post CABG surgery just makes me doubly at risk. For the past nine months, I’ve been at home or at dialysis, with probably less then a dozen other outings: sister’s house, work, last Thursday’s church cell meeting, etc. Not a good start on a new life. I was all gung-ho about recovery a year ago. I seriously thought I would be running 5k or 10k races after a year, but I didn’t count on all the subsequent heart issues like a-fib and pulmonary edema. Now I’m looking forward to another “birthday” when I get a kidney transplant, hoping that will be the “real” start of a new and healthier life.
Crit-Line, Day 2
The dialysis center used the Crit-Line monitor again today to measure my change in blood volume % during dialysis. They think I still have some more fluid to take out, which matches with UCLA’s request for more “aggressive” dialysis. I went into the session at 82.0 kg, a gain of 2.8 kg over Thursday’s ending weight of 79.2 kg. We originally set the UF to 3000 mL over four hours, which is 750 mL/hour. However, the Crit-Line graph showed that there was not much change in the blood volume so we increased the rate to 1000 mL/hour, then to 1200 mL/hour.
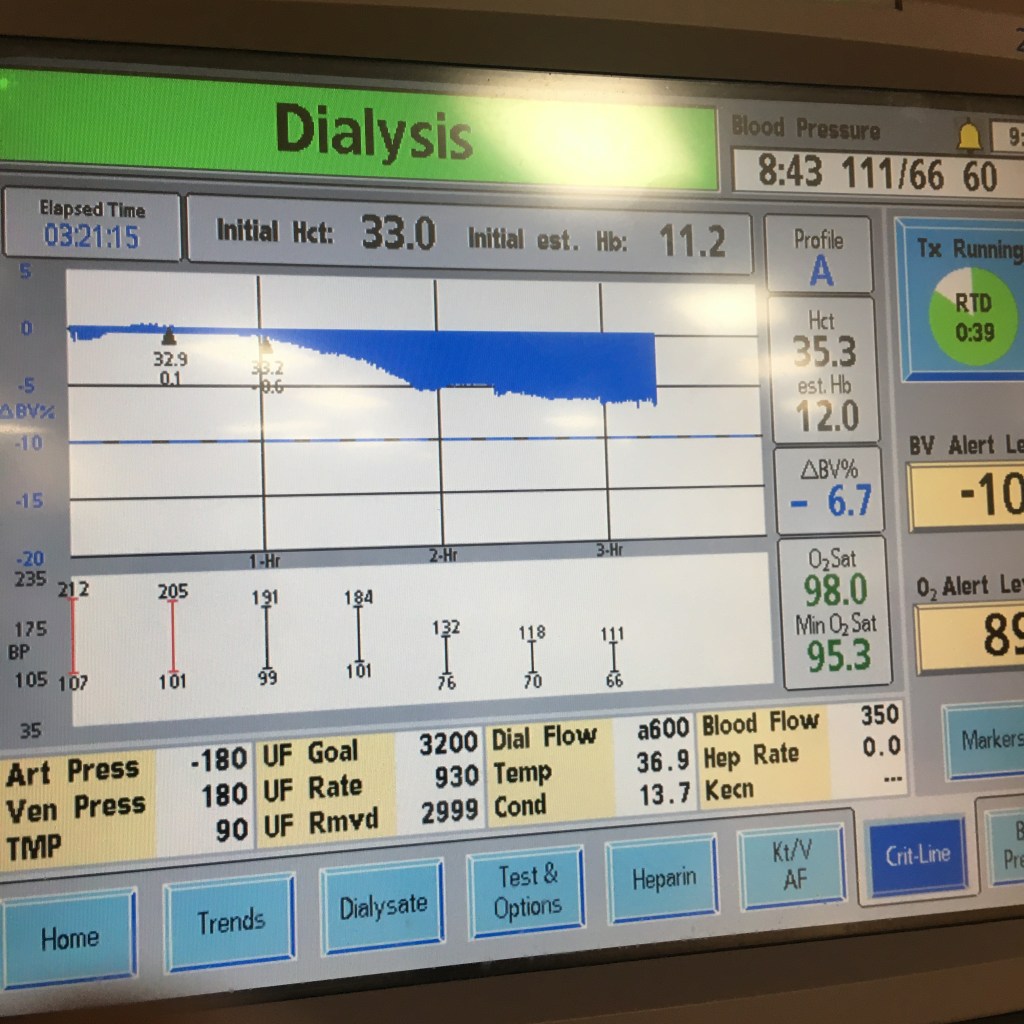
From the photo above, you can see a definite drop in blood volume after the first hour.They ended up taking out 3217 mL of fluids in total over the four hours. You can also see the blood pressure measurements. It starts with a ridiculous 212/107 measurement, but once the blood volume starts dropping, the blood pressure also drops very quickly. At the end of hour 2, blood pressure is down to 132/76, and even lower to 111/66 at end of hour 3. I think my final systolic standing blood pressure was 103. I initially felt fine walking out but got a bit dizzy in the parking lot. I ended up getting some lunch and went to charge my car at the Santa Ana Supercharger.
I do think we’re getting close to getting rid of the excess fluid. My lower legs were on the verge of cramping today during dialysis. Maybe that’s due to the 1200 mL/hour rate. I had read that the UF rate should be kept under 10 mL/kg/hour. At ~80 kg, the maximum UF should be ~3200 mL over 4 hours or ~800 mL/hour. The supervising nurse came by and said that I’ve probably been waterlogged for a few months, and it may take a few weeks to get me back to the correct dry weight.
“Aggressive” Dialysis
I just received a call from my transplant coordinator. After their cardiologist reviewed my most recent echocardiogram, they want me to do another one after some “aggressive” dialysis. I believe the reason was that the last test showed high blood pressure and they want me to try again after some fluid removal. This matches what the Crit-Line thingy showed today, and they dialysis center is already trying to remove more fluid.
However, the instructions seem kind of vague. WTF is more “aggressive” dialysis? You can’t really change the cleaning cycle so I guess we’re all talking about more ultrafiltration or fluid removal. I sent a message to the transplant cardiologist, my local cardiologist, and also my nephrologist asking them what to do. Since this is yet another hurdle on the way to getting a kidney transplant, I want to make sure I’m not being rejected due to some random test result.
Critical Illness Insurance
I talked about my work getting additional voluntary insurance starting in 2017. I’ve signed up for it since the beginning, though I have not made any claims yet. Since I’m coming up to my one year surgery anniversary, I thought I would call Allstate and ask about deadlines. The CSR said they would like the claims within 90 days (!) but may take claims up to a year. I then asked about ESRD and she said that they take the first day of dialysis as the incident date. Well, that’s over four yeas ago so I’m pretty much SOL on that. Even the CABG claim will take a few weeks to get the paperwork complete so I probably won’t get that either. The ESRD diagnosis was supposed to pay out $50k, and $12.5k for CABG surgery. The CSR suggested that I file a claim anyway since I won’t get anything if I don’t file; worst case scenario they reject both claims.
I should have asked this a long time ago, but filing the claim makes the medical problems more concrete. I’m a procrastinator and it’s costing me a lot not to file these claims but I don’t feel like caring. I guess now I know the deadlines, I’m filing the kidney transplant claim (also $50k) as soon as I have it scheduled.
Fluid Removal Lesson
Just got a 10 minute lesson on fluid removal from the head dialysis nurse. There is an attachment on the machine that measures fluid volume in the blood plasma. I think the gist is that fluid is always being transported from cells to tissue space to bloodstream. However, if you can’t make urine, then the fluid stays in your bloodstream, which causes high blood pressure and excess fluid can backup in your organs (e.g, lungs).
This supports my theory that I’ve been losing tissue mass but retaining fluids. By keeping my “dry” weight somewhat constant, I’m actually retaining too much fluid. This was pretty evident a few months ago when I had difficultly breathing and a CAT scan showed ~500 mL of fluid in my lungs. It’s better now since they lowered my weight but it’s probably not enough. My lower leg and ankles are still swollen sometimes and my breathing is not back to 100% yet.
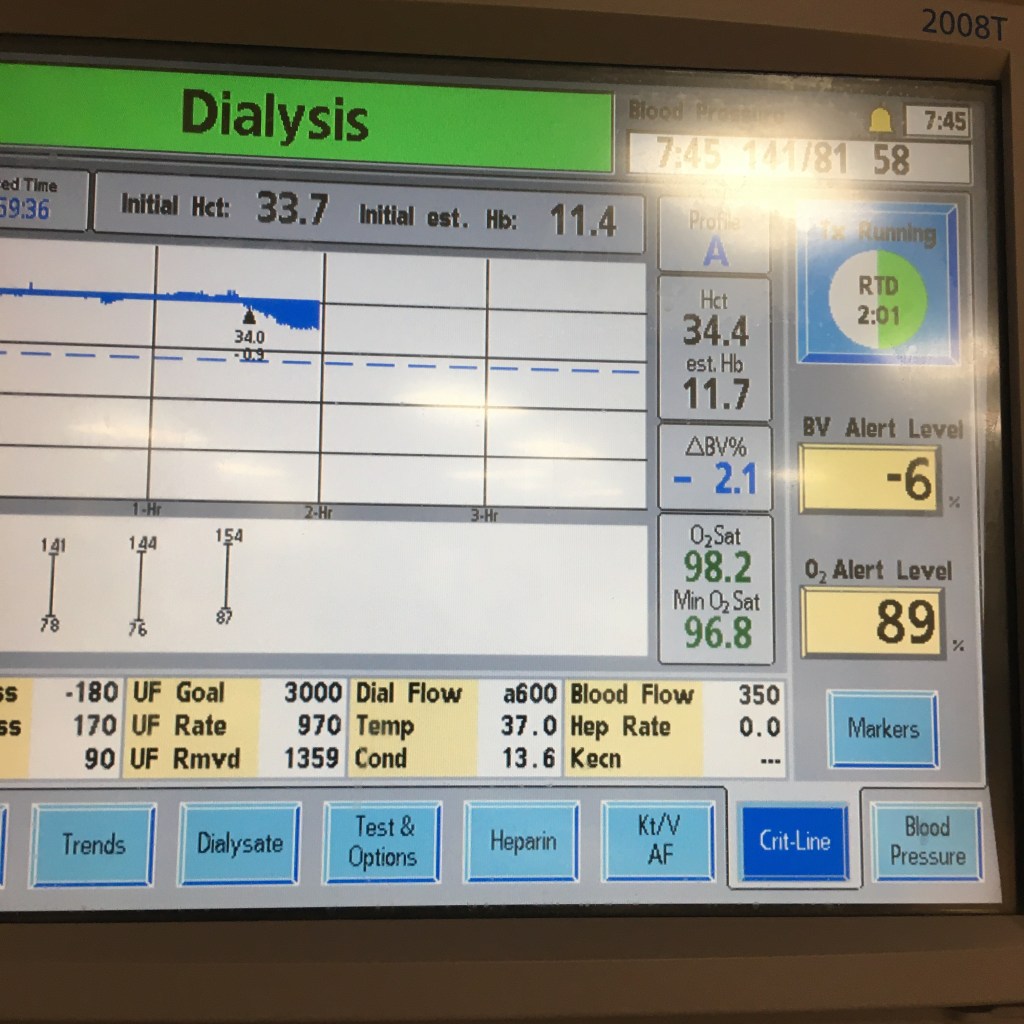
The above is a new screen on the machine that I haven’t seen before. It shows the change in fluid volume in post-dialysis blood. Before the marker on the graph, the change was around zero, which means my body was transporting the same amount of fluid to my bloodstream as the machine was removing. It’s basically saying we need to increase the rate of fluid removal to effectively reduce blood volume. I think the previous rate was 640 mL/ hour, and now it’s up to 970 mL/ hour. You can see the difference in the chart after the marker. My blood pressure is also dropping, which is normal for dialysis. I think the last systolic reading was 157 over something. Previously, since the blood volume was pretty constant and my medication for high blood pressure was being dialyzed out, my blood pressure was actually increasing. This also means that my weight post-dialysis will probably drop some more.
I did ask the nurse why they don’t run this analysis on every patient every session. She said most patients are stubborn and have lots of opinions about their treatment, especially how much fluid to remove. That seems crazy to me; why would I know more about dialysis than the nephrologist/nurse/technician? This device takes the guesswork out of determining the right amount of fluid removal. They’re going to do this a few more sessions to pinpoint the optimal fluid removal rate.
Science!
==========
We had to turn off the ultrafiltration part of dialysis about 30 minutes from the end since I was feeling dizzy, and my systolic blood pressure dropped to 103. I didn’t get a photo of the Crit-Line screen but the blue area was decreasing at the end, and my blood pressure starting increasing a bit. I think the systolic number got to 128 at the end of the session and I no longer felt dizzy. I left the dialysis center at 79.0 kg, which is the lowest weight recorded so far. We’re going to use the device again on Saturday since the nurse thinks there is more excess fluid to remove, but we’re going to start on a higher ultrafiltration rate and lower it over time, instead of starting low and going high at the end. This should reduce the risk of hypovolemic shock.
ER Visit: One Year Ago
On November 11, 2019, I visited my peritoneal dialysis nurse for a scheduled appointment. While I was there, my heart rate was running at 130+. My nephrologist happened to be at the clinic as well so she listened to my heart and suggested that I visit the ER. That led to an EKG and some blood tests, and next thing I knew, I was back on hemodialysis and prepping for heart bypass surgery.
One year later, things are still not back to normal. Most of it has to do with the COVID-19 pandemic, which affected just about everyone. I think I was pretty much recovered from heart surgery after three months off, but then had some episodes of atrial fibrillation and fluid imbalance problems. I also managed to lose about 60 pounds during these 12 months. It’s been a pretty crappy year as documented by all the posts in this blog, but hopefully things will get better post-transplant surgery.
Peripheral Neuropathy 11/9/2020
For the past three days, I’ve had pretty intense nerve pain attacks. Two nights ago, it was the inside of my right foot. Then last night, there were two spots on my left foot. Fortunately, those areas of pain stopped this morning. However, while I was sitting down eating dinner, another attack started on the top of my left big toe. This one is hurting pretty badly now. The pain would last for 2-3 seconds and is increasing in intensity.
I mentioned before that these attacks used to come once a month and last for about 24 hours. Now it seems that there is a new pain area each day. I’m popping Tylenol like candy and usually it has no effect. I basically have to try an fall asleep through the intense pain and hope that everything subsides when I wake up. I don’t know if this is a temporary thing or if I will have neuropathy attacks daily from now on.
==========
Ugh. I guess I rubbed my toe to hard trying to massage the nerve ending. Not only did it not help any, now I have a blister on the top of my toe. In the past, I thought it was because I used a massage wand but just using my thumb will cause a blister too. Fortunately, it’s not too big and on top of the toe and I drained it and put an band-aid over it.
Transplant Social Worker
I just had a video call with my transplant social worker from UCLA. It’s another hurdle in the long path to a transplant. It’s actually the third time I’ve spoken to a social worker from UCLA; each time there’s a potential transplant surgery, I have to go through the entire process. The questions were pretty generic and I don’t think there were any problems or red flags. The only item that came up was having a backup caretaker post-surgery since my mom doesn’t like freeway driving. I spoke to my friend who was a potential live donor and he volunteered to help out. I gave his contact info to the social worker so I think that part is done. I just have to wait a month for the colonoscopy appointment.
Medical Issues 11/8/2020
It’s 2:35 am and I can’t sleep, mainly because my peripheral neuropathy is acting up again. I’m getting intermittent pain on the inside of my right foot. It started about an hour ago; I just took some Tylenol PM to see if that will help. Since I’m up, I thought it would be a good time to update my medical issues list:
- ESRD: the end may be near; my sister was accepted as a donor at UCLA and all I have left is a colonoscopy; there is some concern about some recent heart tests (Lexiscan stress test and echocardiogram) but my cardiologist thinks I should be fine for a kidney transplant
- Dialysis access: it’s been mostly okay after the fistulagram procedure; the techs still have some difficulty inserting the needles on some days
- Cardiac rehab: if UCLA is okay with my heart test results, then I don’t think I will go back to complete the program
- Peripheral neuropathy: since I haven’t been walking due to excess fluid in the lungs and getting that huge cut in my toe, I think the neuropathy attacks are increasing in frequency; I’m sitting here typing at ~3:00 am because an attack is keeping me awake now
- Back pain and pressure in chest: there is still some fluid in my lungs but much better since dialysis is lowering my dry weight and removing excess fluid
- Minimal urine production: no change
- Insomnia: the breathing issue is much better but most nights the numbness and pain in my foot is keeping me awake
- Dental issues: mostly done; probably have some cavities to take care of but those can wait until next year
- Endocrinologist: next appointment in December; A1C test results still in the “n0rmal” range
- Lump in left leg: no change
- Constipation: no problem now; having pretty regular bowel movement
- Ophthalmologist: still shows some retina damage from before but no real change from year-to-year
The huge cut in my foot/toe was a complete surprise. I guess I’m just unlucky. Dialysis was taking care of my excess fluid problem and I was getting ready to start walking again but that was delayed so my foot can heal. I have an appointment with the podiatrist in about a week to see if the cut is healing after he took out the sutures.
COVID Travel Restrictions
I saw this behind an exam room door during my colonoscopy consultation meeting:

I’m sure it’s pretty old since it asks about travel to China, South Korea, Iran, Italy, or Japan. That was the first wave COVID infection and seems to correspond with a Trump travel ban in March. If we were to update this list today, it would probably be a list of states in the US instead.
Taylor Guitar
I purchased a Taylor acoustic guitar many years ago. It was a special edition 414ce-L4. I purchased it at a local music store and I think I paid about $1,600 for it.

The EXIF data on the above photo says it was taken in January 2004. That seems like an entire lifetime ago. I was still pretty healthy and still married. The photo was taken in the living room of my house in Brea. I’ve since sold the house and moved twice, but I still have the guitar. For the past 10 years, the guitar has been sitting out on a guitar stand. I helped lead worship at my old church for several years and would practice/play the guitar several times a week so it got a lot of use. When I was in the hospital for two weeks post-surgery, my parents reconfigured my bedroom and packed away the guitar. I haven’t seen it in about a year. I thought about getting it out again during the COVID lockdown but never got around to it.
==========
I also got some email advertising from Musician’s Friend. I bought some pro audio equipment from them so I guess I’m forever on their list. I just looked at their website and the current version of my guitar is $2,400. Not sure why it’s more expensive at the music store than the Taylor website.
Proposition Results
California is a weird state. It’s a solidly blue (Democrat) state in every election. The Democratic Party has a supermajority in the state legislature, and a lot of historically Republican districts are voting Democrat, especially Orange County. However, if you look at some of the early results for ballot measures, the Democratic Party are big losers.
From the California Secretary of State website, results as of 10:40 am on 11/3/2020:
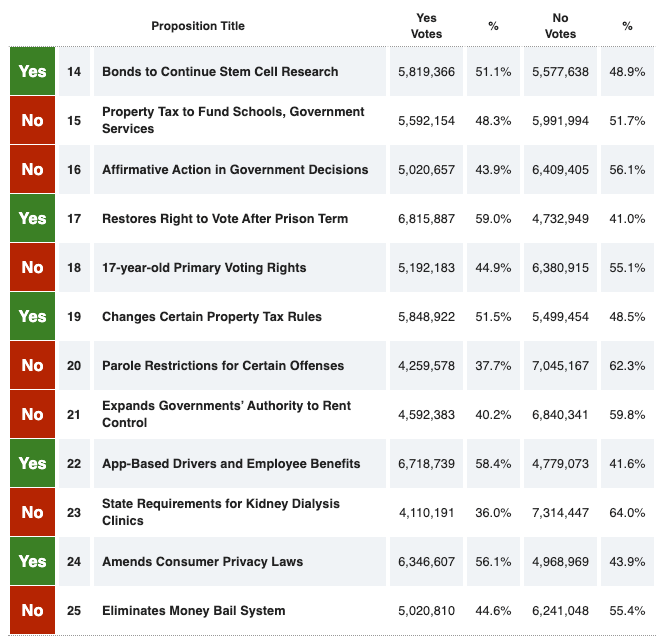
Two of the most contested propositions in terms of funding are 22 and 23. If you look at Ballotpedia, you can see that the Democratic Party were against 22 and supported 23.
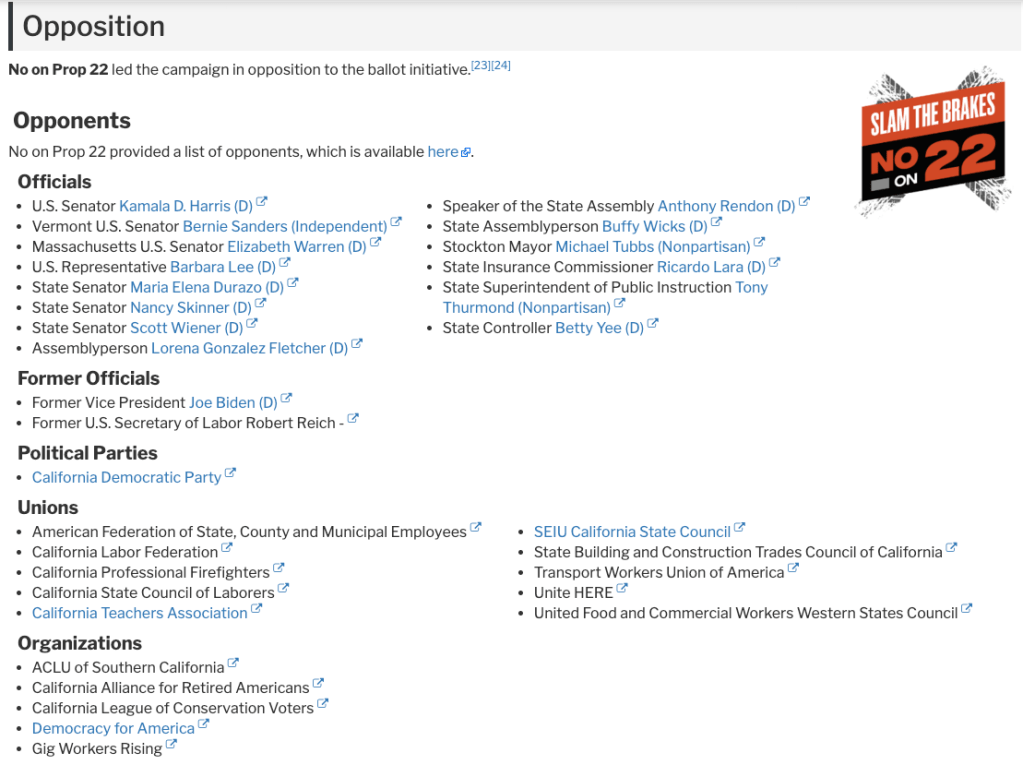
Both these propositions have clear union positions, which is probably why it’s heavily partisan. Even worse, proposition 16 seems to be losing as well. Affirmative action is a bread-and-butter Democrat issue. The support list is huge with literally every Democrat politician supporting the overturn of proposition 209.
So what is going on? Why can’t a super-blue state pass ballot measures supported by the super-majority party? An even more fundamental questions is why can’t the state assembly pass these as laws? I guess they did for gig workers but proposition 22 overturns it. Maybe the voters just don’t like the Republican candidates but also don’t like the Democratic agenda.
Here is the Democratic Party endorsements for ballot measures in California. Compared to the partial results above, they’re not doing very well. Looks like it’s four out of eleven so far. Again, that seems weird to me since California is supposed to be a Democratic stronghold in politics.
Fistula Update 11/3/2020
Election day!
At the end of the dialysis session, after the tech removes the needles, I usually have to sit there and hold some rolled-up gauze on the needle sites to stop the bleeding. Today, the fistula bled a lot. It was probably the most I’ve ever seen of my own blood.
Since I have to sit there an hold the gauze for 10-15 minutes, I’m usually reading Reddit on my iPad. Normally I’m not looking directly at my arm. Today, I felt my arm getting warm which is unusual. When I looked over, there was a huge pool of blood under my arm. I quickly got the tech over and she managed to change the gauze. I then applied pressure again but it was still bleeding. The tech thinks my vein “rolled” away from the gauze while I was applying pressure so she stood next to my chair and held the gauze for 10 minutes. My fistula did stop bleeding after that but I wonder how much blood I lost.
I ended the session at 79.2 kg. The nephrologist lowered my dry/ideal weight again to 79.5 kg so I’m still losing weight, though not as much as the weeks right after surgery.
Colonoscopy Consult
I went to meet with the nurse practitioner yesterday. What was supposed to be a 15 minute meeting turned into over an hour. I arrived 10 minutes early having completed a bunch of forms online. Of course, they still had forms to fill out so I spent 15 minutes filling them out. Then I waited 10 minutes for someone to call me just to bring me to an internal office where I sat for another 10 minutes. So close to 25 minutes after my appointment time, I finally get to talk to the nurse. She was really nice though and explained the procedure briefly. She also asked if I would participate in a study where they draw some blood and look for markers that match up to the colonoscopy results. After being sick a lot, I now agree to almost all studies since why not? Anyway, that was another 20 minute wait for the study nurse to interview me. The second nurse also took blood samples… about 8 test tube worth… with a very slow butterfly needle. Not sure if she’s also a phlebotomist but it took many pokes to get the blood going. Finally, they schedule the procedure and it’s not until December 15th. Ugh. That means likely there is no transplant this year. <sad face>
One tiny positive is that the study pays! I can’t remember exactly how much but it was ~$100 to $150. Better than nothing I guess.
Missing Glasses (updated)
Weird.
I have two pairs of glasses. Prior to this, I had a pair of trifocals since I can’t see near or far. That got changed to two pairs of glasses: one for driving, and one for computer work. As it turned out, neither one is good for close up reading so I usually take off my glasses when reading stuff on my iPad or iPhone. However, my day-to-day glasses are the ones designed for computer work.
Yesterday, I spent a few hours reading a novel on iBooks. I thought I left my glasses on my pillow but when I took a reading break, I could not find my glasses. I looked everywhere in my bedroom but could not find it. I ended up going to my car to get the driving glasses but I can’t see closeup well with them so it’s not helping that much. To do work, I have to take off my glasses and get within six inches of the computer screen to see clearly.
I’ve been looking for my glasses since last night, and now my parents are looking too. They should be in my room since I can’t really see without them, and don’t remember/can’t imagine leaving the bedroom without them.
==========
Updated: 10/29/2020 3:40 pm
Found! They were lying on the floor next to my bed, on top of a bunch of wires. I have a six port USB power hub that’s plugged into an AC outlet. There are lots of USB cables attached to it and all the wires were jumbled together. My glasses were just lying on top of the mess. I swear I checked there last night, and both my parents looked there as well. Great camouflage, I guess. I only found them because I was untangling some of the wires to plug my phones in. I felt rather than see the glasses. So weird.
Echocardiogram
I had an echocardiogram done this afternoon, at the request of my cardiologist and UCLA Transplant Center’s cardiologist. The procedure is basically a heart ultrasound and it only took 15 minutes. Weird that such a short test can affect the rest of my life.
The tech had me take off my shirt and lie down on an examination bed. Most of the test was done lying on my left, which is not that great for me. Even almost a year after the bypass surgery, I still feel pressure when I lie down on my left. I think I mentioned in a previous post that my cardiologist wanted to double check the LV EF (ejection fraction) number since my latest results from the Lexiscan was pretty low. She said the Lexiscan EF results were not as accurate as an echocardiogram; let’s hope that’s true and the results are better this time.
Another Heart Test
During dialysis, I got a phone call from my cardiologist’s office. I had asked them to send in the results of my Lexiscan heart stress test to UCLA Transplant Center. UCLA’s cardiologist (I’ve seen him before in April) then requested an echocardiogram (echo). My transplant coordinator at UCLA also called me a bit later about the same issue so I told her the echo was already scheduled. I guess things can move fast when they want to. My echo test is this coming Thursday at 1:45 pm.
I’m not sure how to feel about this. This one test has been a mini-emotional rollercoaster. Initially UCLA said I didn’t need a heart stress test since I had bypass surgery. This was confirmed by my April appointment with UCLA’s cardiologist. After a phone meeting with the transplant center director, they now say they want a stress test. I was still okay since I passed the same test in 2016 with a “bad” heart. After the results came out, I wasn’t so sure since my LV EF was <40%. For a few weeks, I was sure that would rule me out for a transplant for life. Then my doctor friend said that number wasn’t too bad, and I could probably raise it through exercise. Good thing I just got a deep cut in my foot. My cardiologist then called to explain the test results and her comment that she didn’t see anything that would prevent a transplant made me feel optimistic again. Next, I find out that UCLA never received the test results so I asked my cardiologist office to send them again. Now I feel conflicted since it’s good that I wasn’t rejected based on the heart stress results, but the fact that they want another test worries me again.
Now multiply this by 100 and you can get a sense of my feelings and emotions over the past 4-5 years as I found out about my ESRD condition and starting dialysis.
Fistulagram Medical Claim
Got a statement of benefits from my work insurance regarding my fistulagram procedure on August 21st. The whole thing was billed at $14,261, and the Medicare rate was $5,744. My work paid 20% of that, which was $1,149. Again, not really knowledgeable about medical costs so I don’t know if that’s a fair price. I did spend a bit of time in the hospital, and was in an intervention radiology operating room with several OR nurses. However, this only covers the hospital portion. I’ll probably get another bill/claim from the vascular surgeon. Some of the line descriptions are not very detailed: Outpatient surgery, Medication, Medical equipment and supplies, etc. I wonder if I asked, someone (hospital, Medicare, Blue Shield) will send me a more detailed statement.
Also, I did a drive-thru COVID-19 test on August 18th, prior to the procedure. That was billed at $65 and the reduced Medicare cost was $33.72.