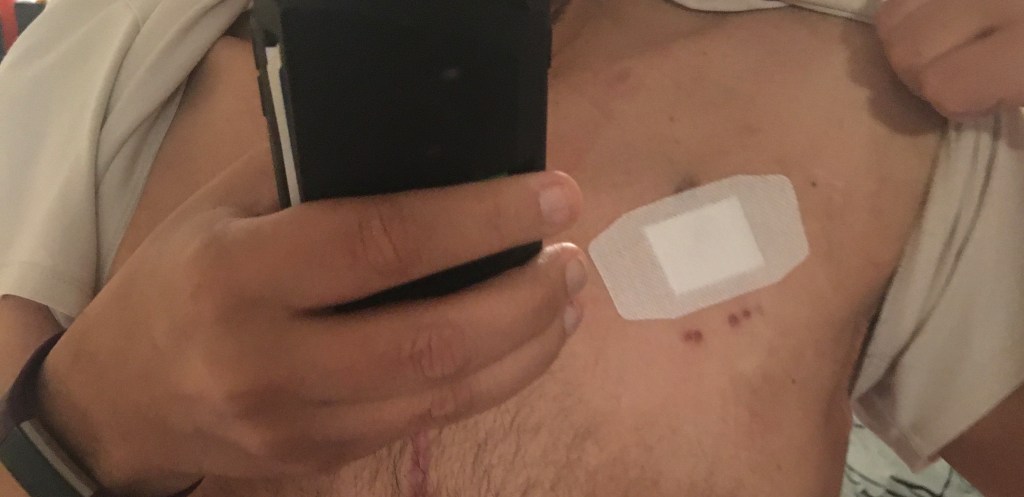
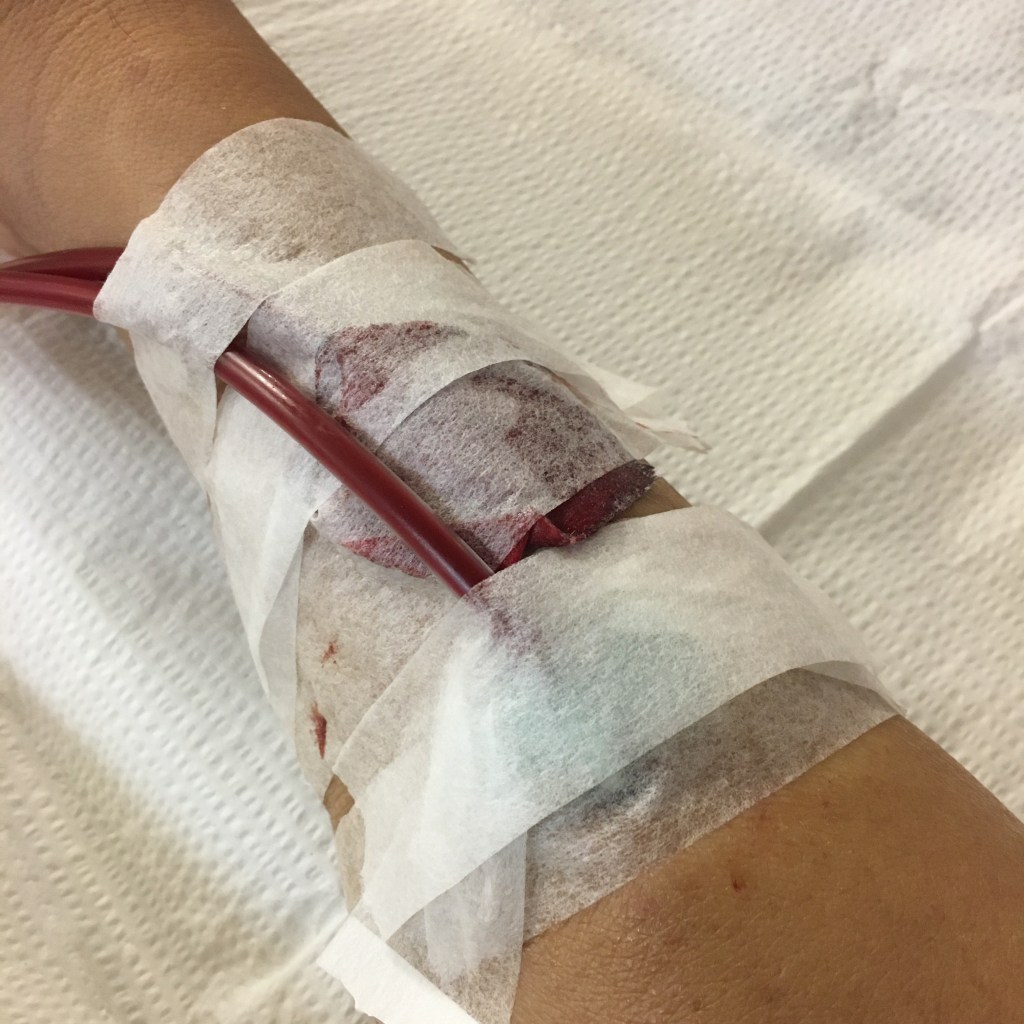
Second chest catheter removed. It was much easier than removing the first one in the hospital. I went into the doctor’s office, sat in a reclining chair, and the nurse laid me flat. The only problem was she stuck a pillow under my back so to arch my back, but that made breathing 100x harder. I think I was going to pass out a few times. Then the surgeon came in with his assistant, who I’ve met several times. I think the surgeon was more interested in my fistula that he worked on then the catheter (he didn’t put that in). He told me the assistant will remove the catheter, and that I need more fluids taken out since my ankles were swollen. OK, thanks. He’s got to know I’m a dialysis patient and there are literally a team of people watching for edema in my legs.
The assistant, let’s call him “J”, gave me several shots of lidocaine, the wonder local anesthesia, and proceeded to cut the sutures holding the catheter in. I think some of the flesh grew in around the catheter cuff so he had to cut around that too. Then J gave a hard tug, and it was out. Only problem? No one mentioned to him that I was on a blood thinner, and of course no one told me to hold the medication. Blood started squirting out of the opening. I didn’t see this but J told me later. He had to grab a lot of gauze and bandage to stop the bleeding, even asking me to put pressure on the wound. Good thing I didn’t pass out from the lack of oxygen. I was already breathing hard; putting pressure on my chest just made it even worse. Finally, after three gauze changes and lots of pressure bandage tape, the bleeding stopped and I was allowed to get up… and breath. Even thought J tried to wipe it down, there was quite a bit of blood on the chair. After dialysis with the fistula though, I was used to it. No pics this time, I was too busy trying to breath and not pass out. Here’s a photo after the previous catheter was removed if anyone is interested. I assume this one was similar; I didn’t even look afterwards.
Finally, they let me get up and leave, after giving me an instruction sheet. One of the item says: “Do not lay flat for 12 hours after catheter removal to reduce likelihood of bleeding.” Arg! Why did they schedule me for a 4:30 pm catheter removal, knowing that I have to sit upright until 5:00 am the next morning?! I can’t lay flat anyway but they didn’t know that. Other points are pretty normal post-op stuff.
So, another tiny chapter in my life comes to a close. I kinda like the catheter versus the fistula, even though I couldn’t take showers. I heard other people do shower with waterproof tape, bags, and other homemade contraptions to keep the catheter dry. I’m too nervous to try. Maybe that’s why I’ve never gotten an infection after 2.5 years of using the chest catheter. Supposedly I can take a shower after 24 hours, even if the hole in my chest hasn’t fully closed. yet. Hmm… I think I’ll wait. No point having shower water running through a hole and into your chest cavity.