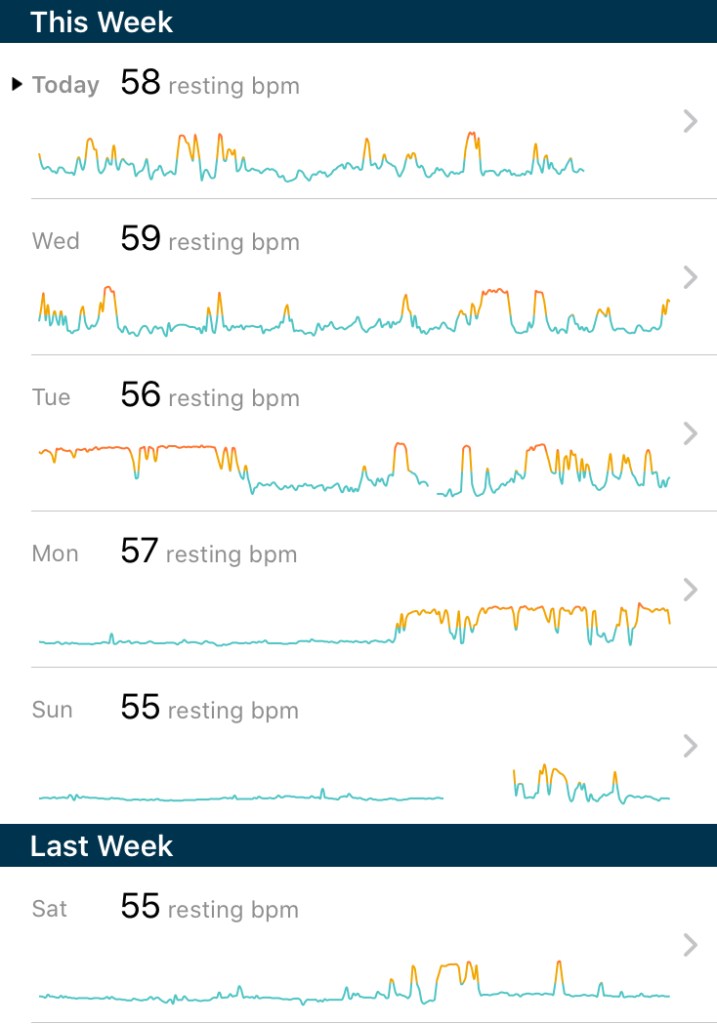
I couldn’t sleep at all this morning. Between anxiety about the cardioversion procedure and chest pain/pressure, there was no way I was going to fall asleep. By staying up, I noticed that my heartbeat was pretty regular at 61 bpm since midnight. When 8:00 am rolled around, I called the cardiologist office to ask what I should do. The receptionist took a message and said my cardiologist would call me back. Actually, during the call, my a-fib started up again. Dang it.
I ended up going to the hospital at 9:30 am as scheduled. My sister dropped me off since they were not allowing visitors for outpatient procedures. Check-in was pretty efficient; they came out with completed paperwork so I didn’t have to talk to the admitting person for very long. On the way back to pre-op, I saw my nephrologist doing rounds at the hospital. She was surprised to see me. I thought I was a bad sign I’m recognizing random doctors walking around in a hospital.
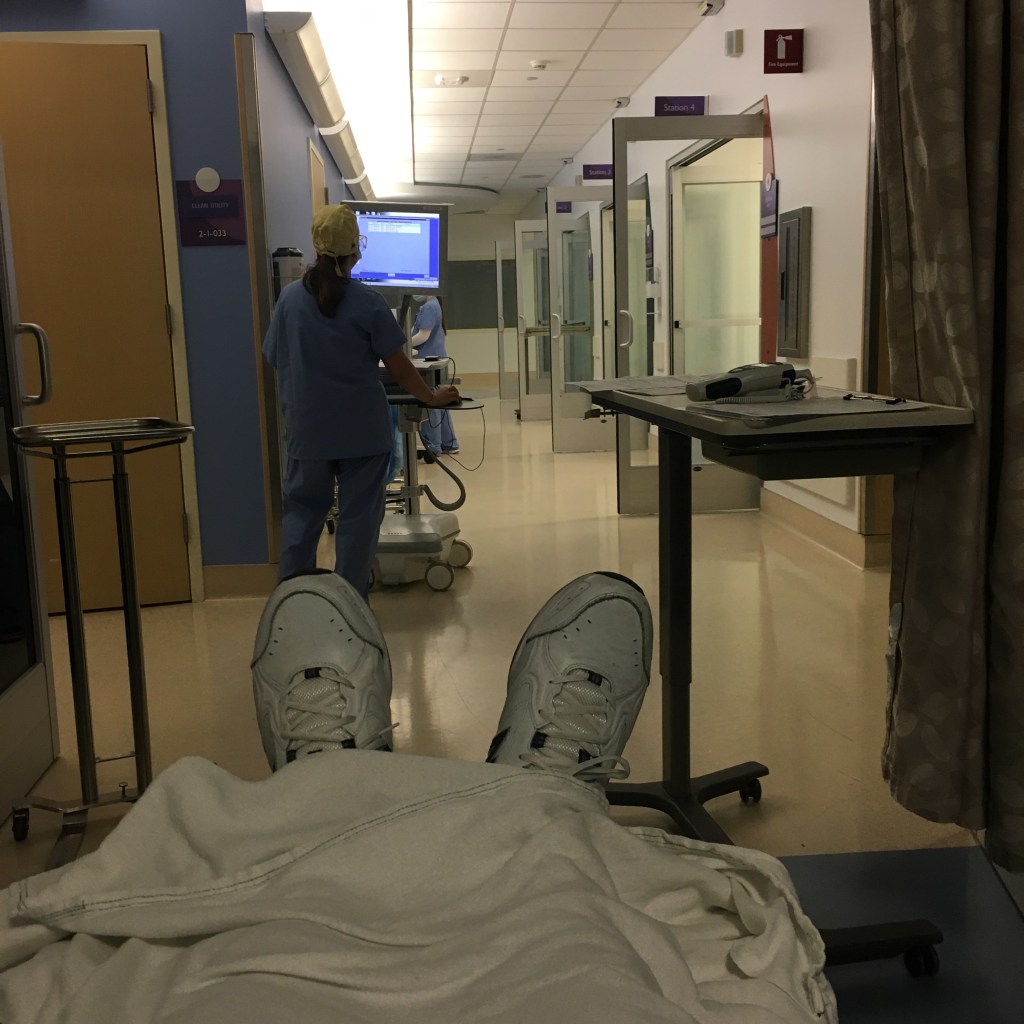
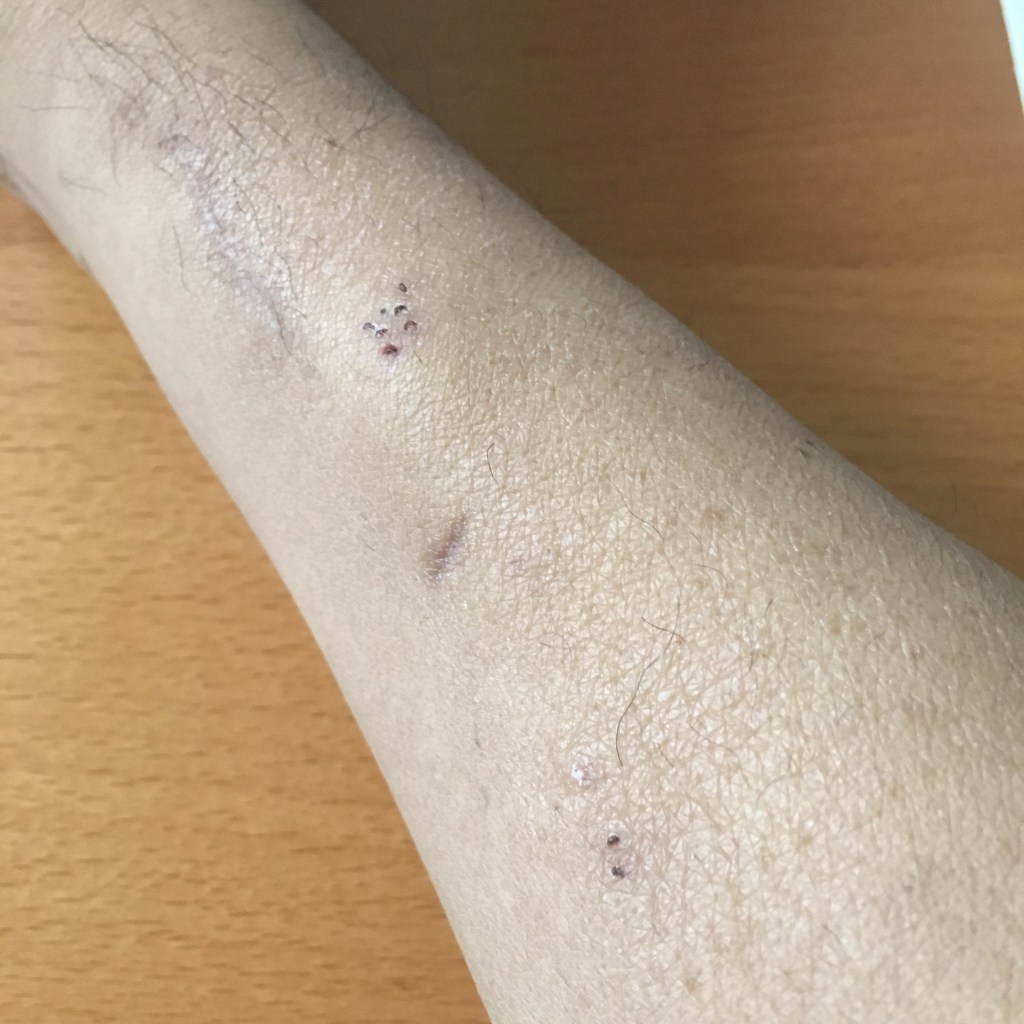
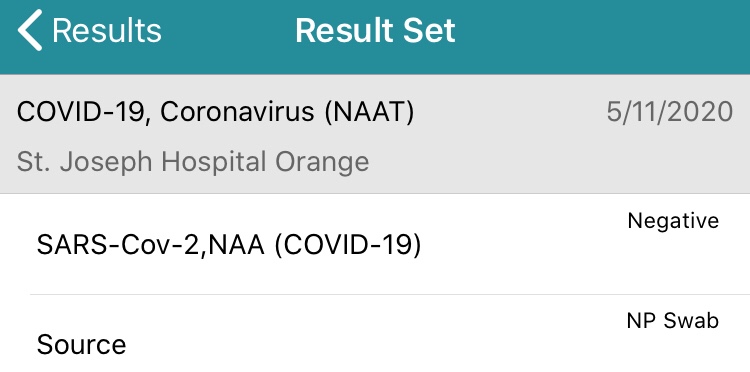
The first thing they did was to get a swab for a COVID-19 test. I just had an antibody test done Friday but this was the antigen test so the nurse crammed a swab way up my nose until it felt like she was digging out some brain matter. Ouch! Thankfully it came back negative. They also drew blood for labs. Since I have a fistula in my right arm, they were limited to the left arm only. The first nurse managed to draw enough blood but took several tries. Then she tried to put in an IV but failed so another nurse came and did it after several tries. Later they said my blood sample clogged and they needed to draw more blood. The IV seemed to be one way (in only) so three nurses tried 10+ times to put in a butterfly needle but failed. My left arm was covered with gauze and bandages. Finally they called the lab for a real phlebotomist. With about 15 minutes prior to the procedure, my cardiologist showed up and the nurse said labs weren’t done because they could not draw blood. The cardiologist said, “I saw the results at my office.” Turned out he original draw was fine. I even had the results on my patient portal app. I got poked those 10+ times for nothing.
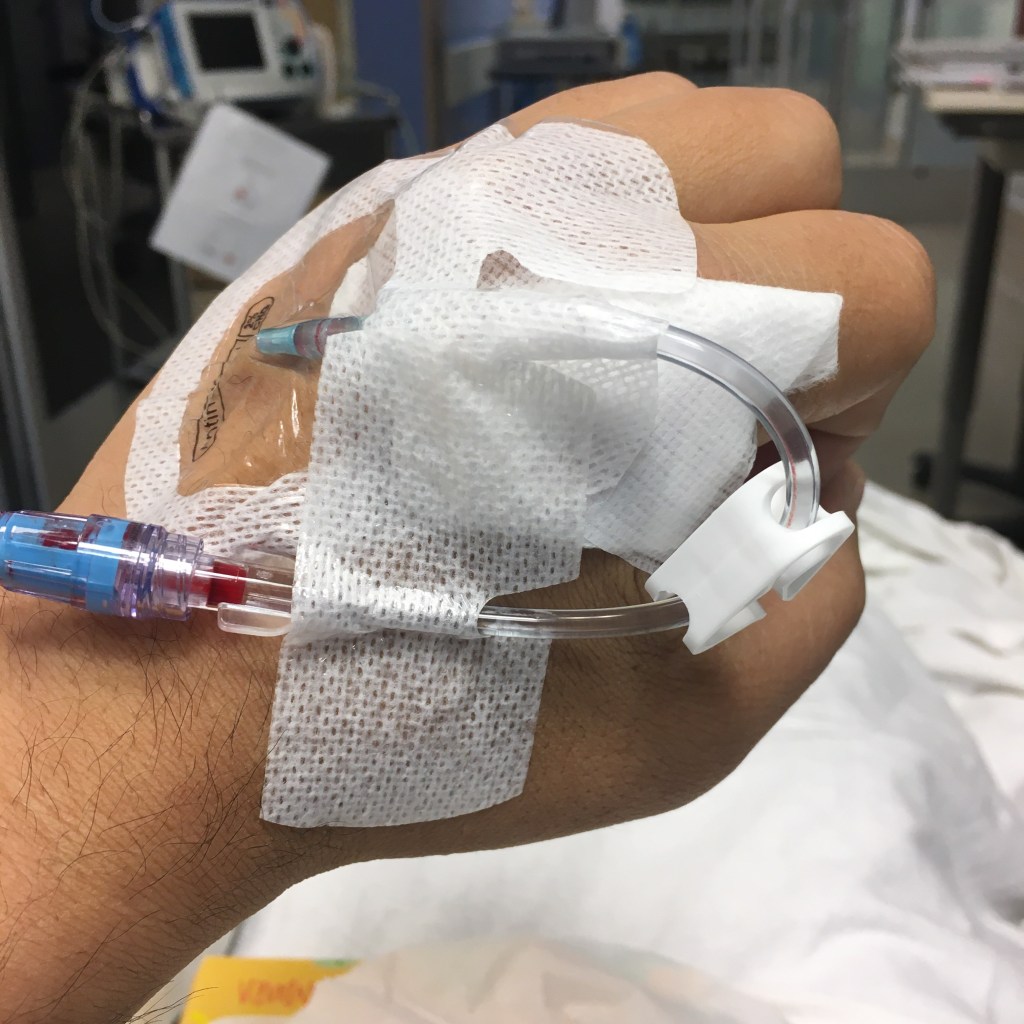
Anyway, it was pretty smooth after that. Cardiologist said she was going to set the machine at 150 Joules; not sure if that’s a lot or not but seems to be similar to a defibrillator. The anesthesiologist came and put me to sleep at around 1:00 pm and I woke up right before 2:00 pm in the post-op recovery room. The nurses there gave me some juice, crackers, and peanut butter since I haven’t eaten in 12+ hours. My sister picked me up at ~2:30 pm so I was at the hospital for a total of six hours. I went home and took several naps, probably due to the anesthesia, and heartbeat has been fine so far.
My cardiologist also stopped my Metoprolol medication so hopefully the Multaq can maintain the steady heartbeat.