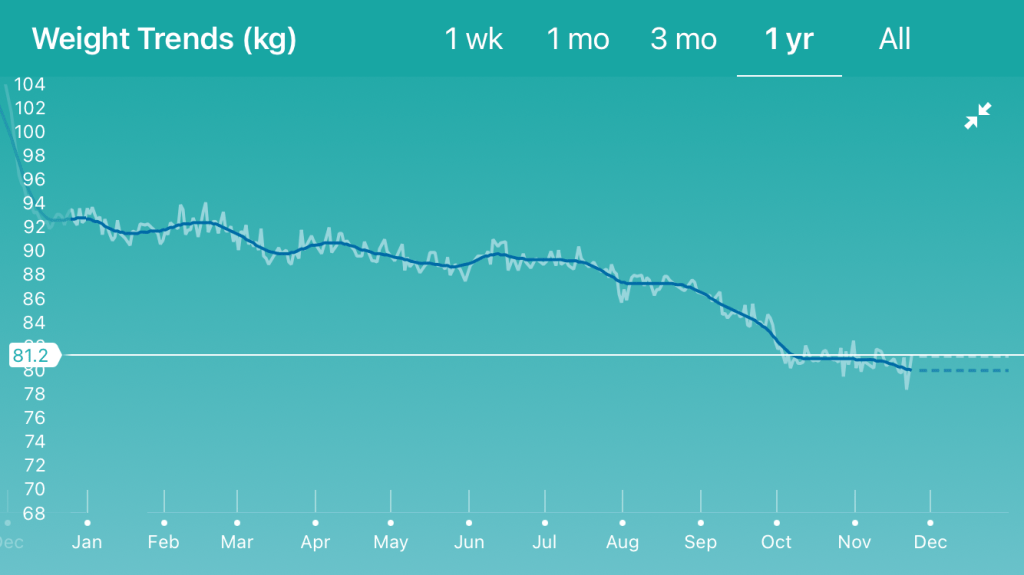
I just got home after today’s dialysis session. Due to New Year’s Day being on Friday, the weekend schedule was shifted back one day. As I mentioned before, my weight was pretty high. Even after removing my thick jacket (but leaving my shoes on), the scale said 83.5 kg. I usually take 0.5 kg off for miscellaneous clothing but I cheated a bit more and told the tech I weighed 82.5 kg. That means I had to cheat at the end weigh-in too. Even at that weight, the tech decided that we would remove 3,800 mL of fluids, probably the most they’ve tried during one session.
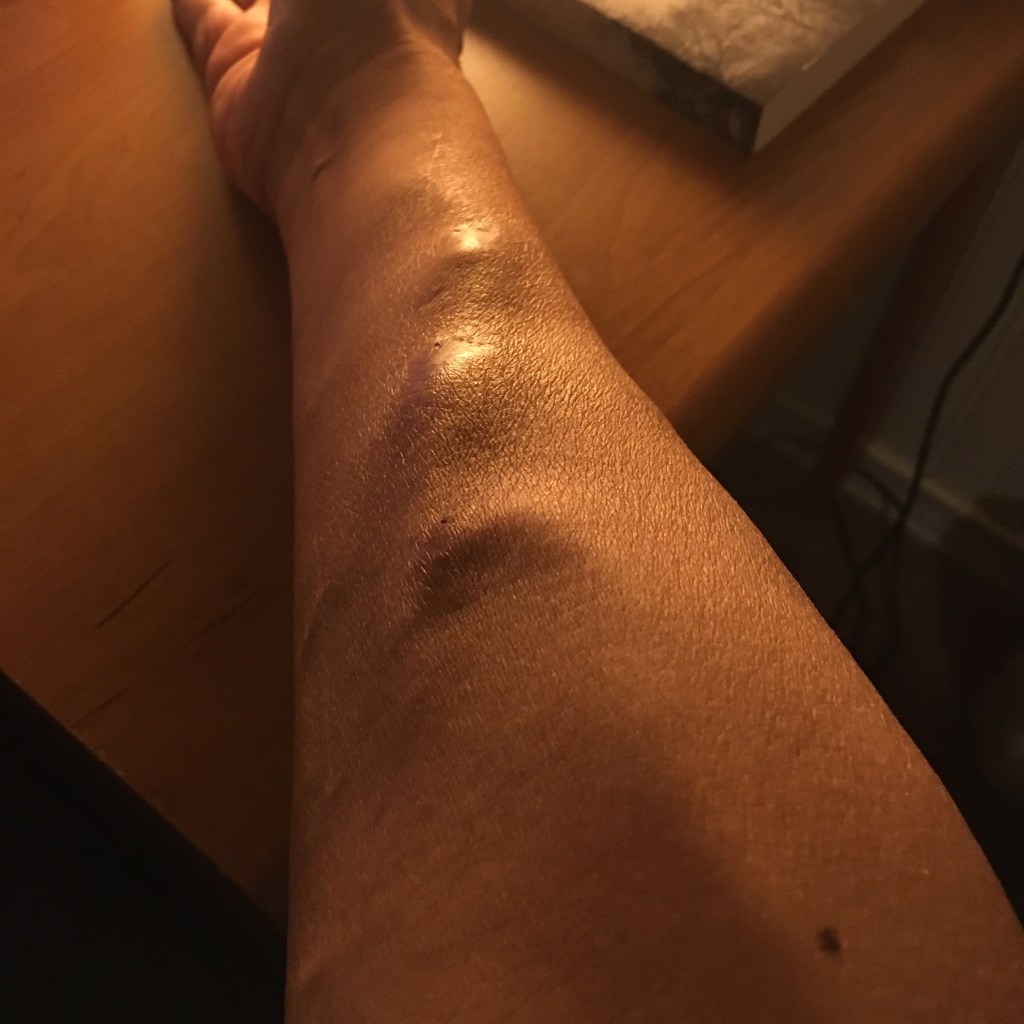
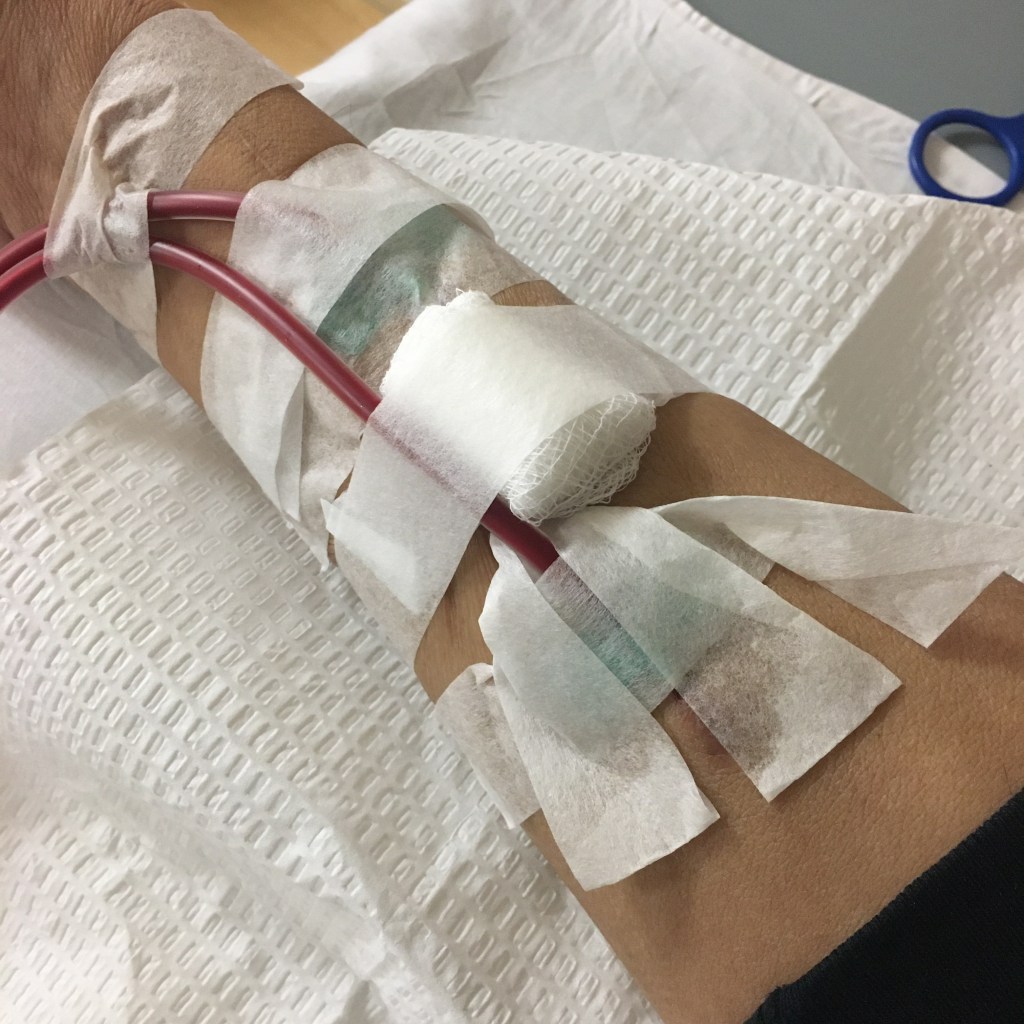
Right at the beginning, there was a problem. The arterial needle didn’t go in that smoothly, and it hurt really bad. The venous needle was a bit better but there was a dull pain in my arm that wouldn’t go away. After about 30 minutes, the tech decides to move the needle since the pressure was wrong, and it hurt a lot worse. He ended up removing the arterial needle and jabbed me further up the arm. Initially, he missed the vein, but was able to hit in with a second needle. He jokingly said he was praying. Not sure how much of it was serious.
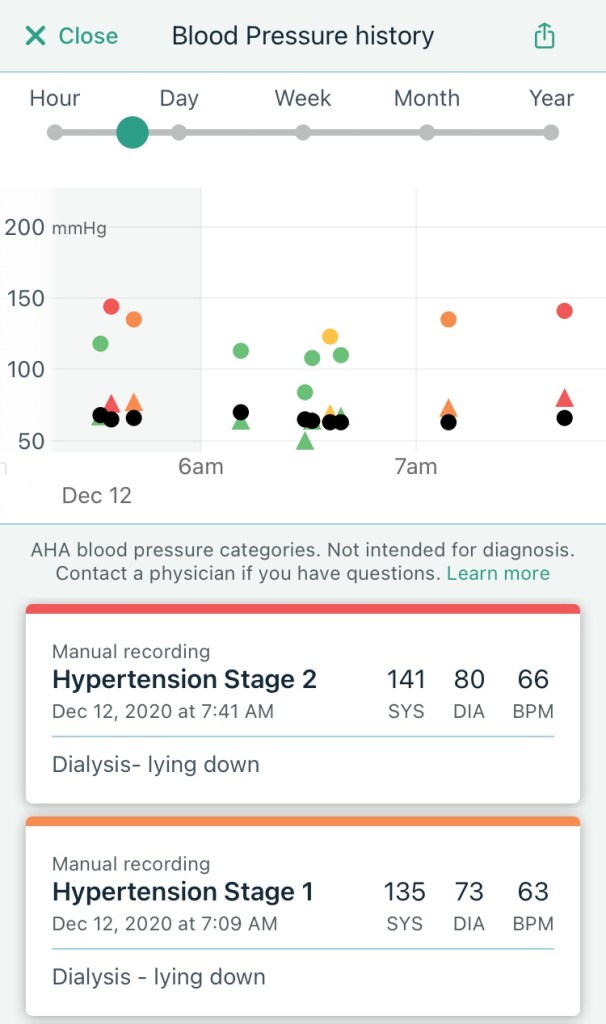
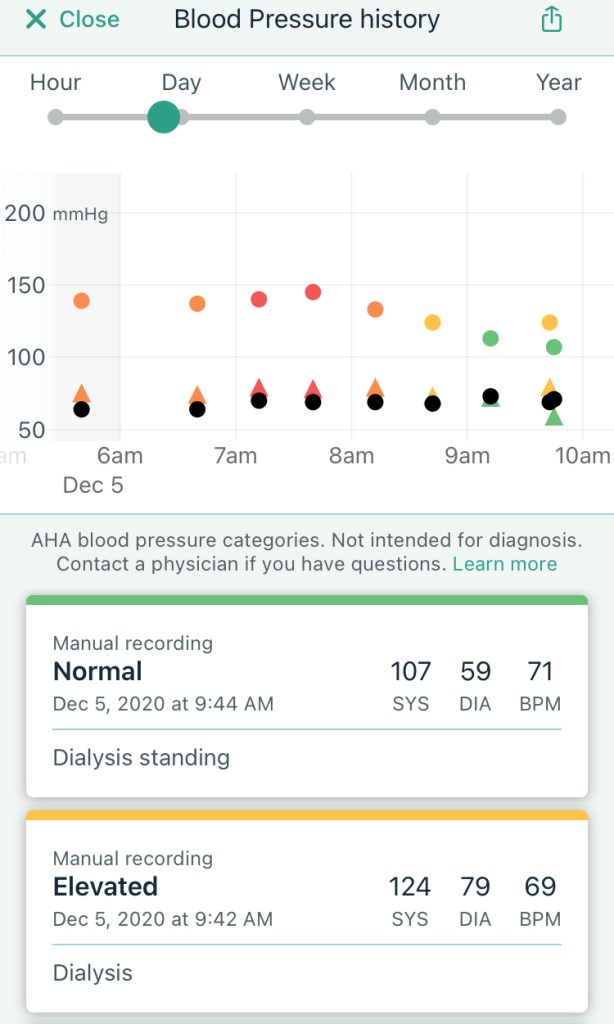
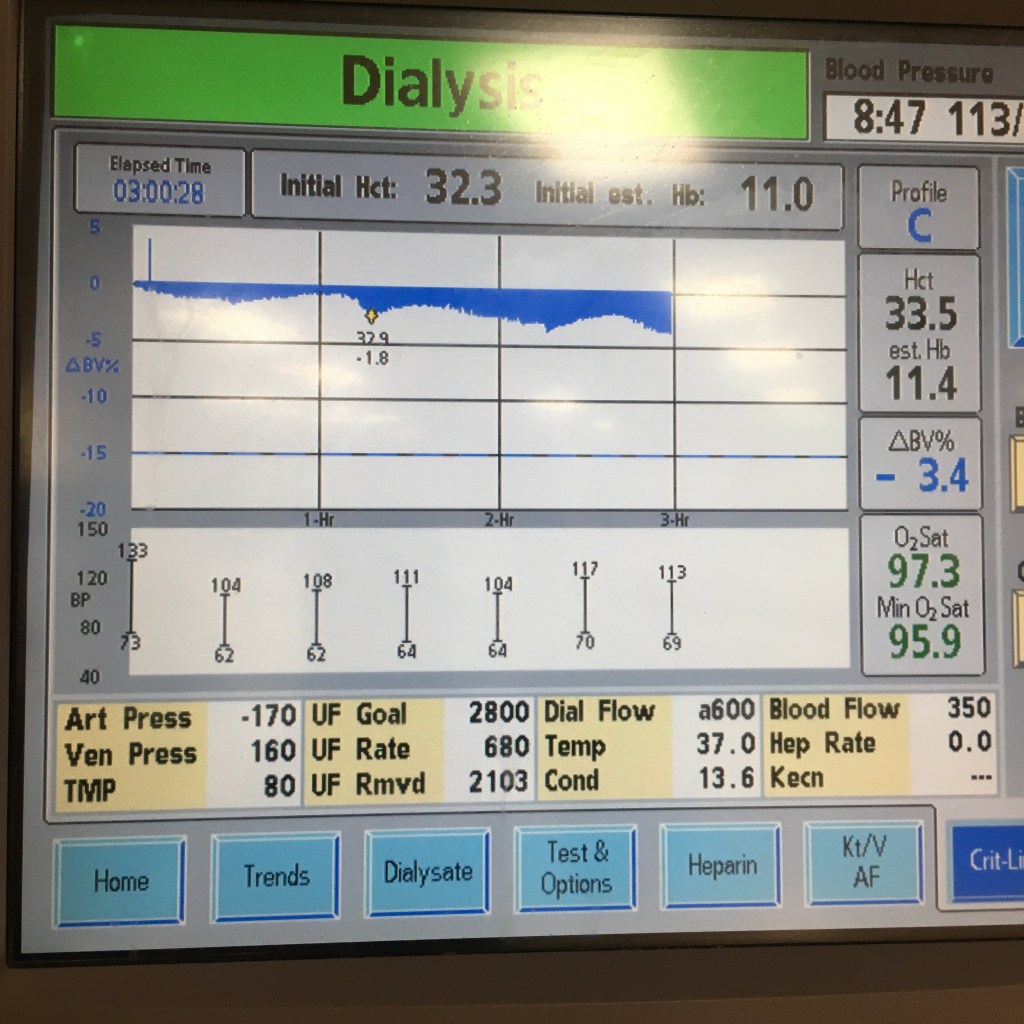
I started getting dizzy around the two hour mark. Both my feet were super numb for some reason but I tried to lie flat in the chair to raise my blood pressure. I guess it worked okay since I was averaging 140/80, even as the machine eventually pulled out 3,732 mL of fluids. When I stood up at the very end for the final blood pressure reading, I almost fell over, and the reading was 85/50. Not good. I took a few sips of water, waited five minutes, and tried again. This time it was 104/70 (or something) so good enough. Walking out, I was still pretty dizzy but felt better once I sat down in my car. The weight reading was 80.1 kg, which was 83.5 kg – 3.7 kg + a few sips of water. I ended up telling the tech that I weighed 79.2 kg so I have to watch what I eat/drink for the next few days. Of course, I was starving and stopped by Raising Cane’s to get four chicken fingers a la carte. No drinks. I ate them while driving home. They were super hot (temperature) and tasted awesome. I think I should get a job there after retiring from my real job. I leave you with a chicken finger video.
==========
Ugh, so tired. I think I woke up for a bit at 2:00 pm but I slept until almost 7:00 pm. Meanwhile, two of the dialysis needle insertion points are still bleeding, visible through the band-aids. I’ve gone through four of them already.