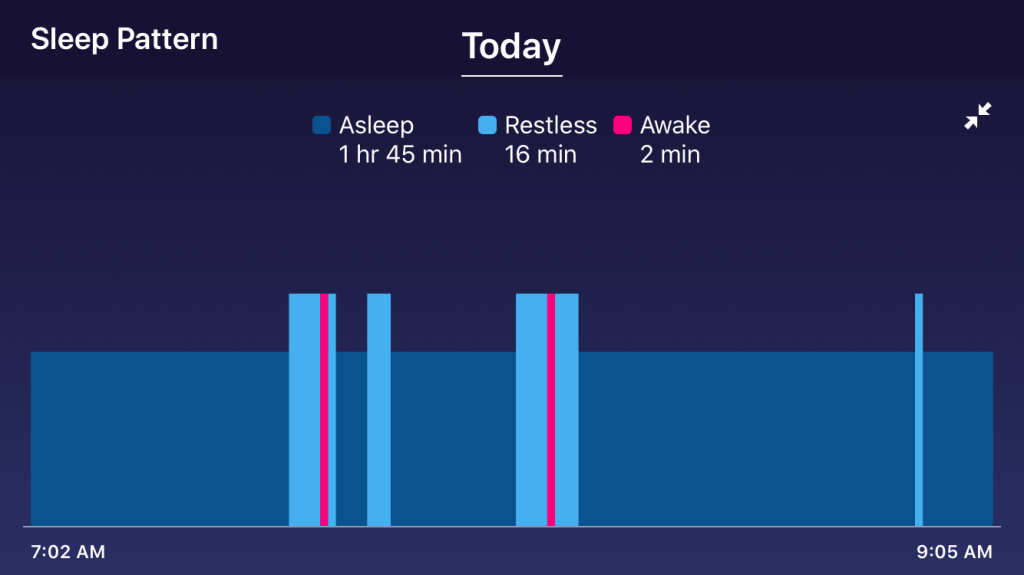
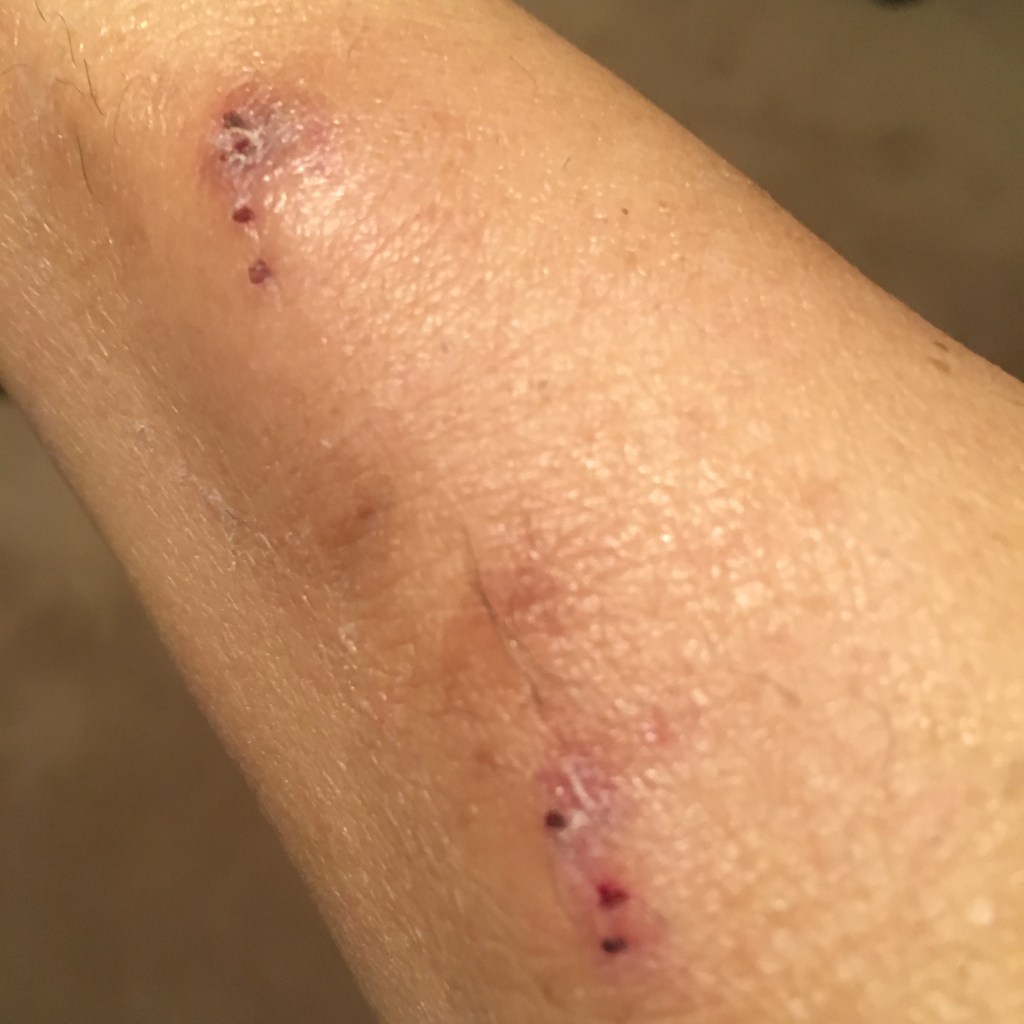
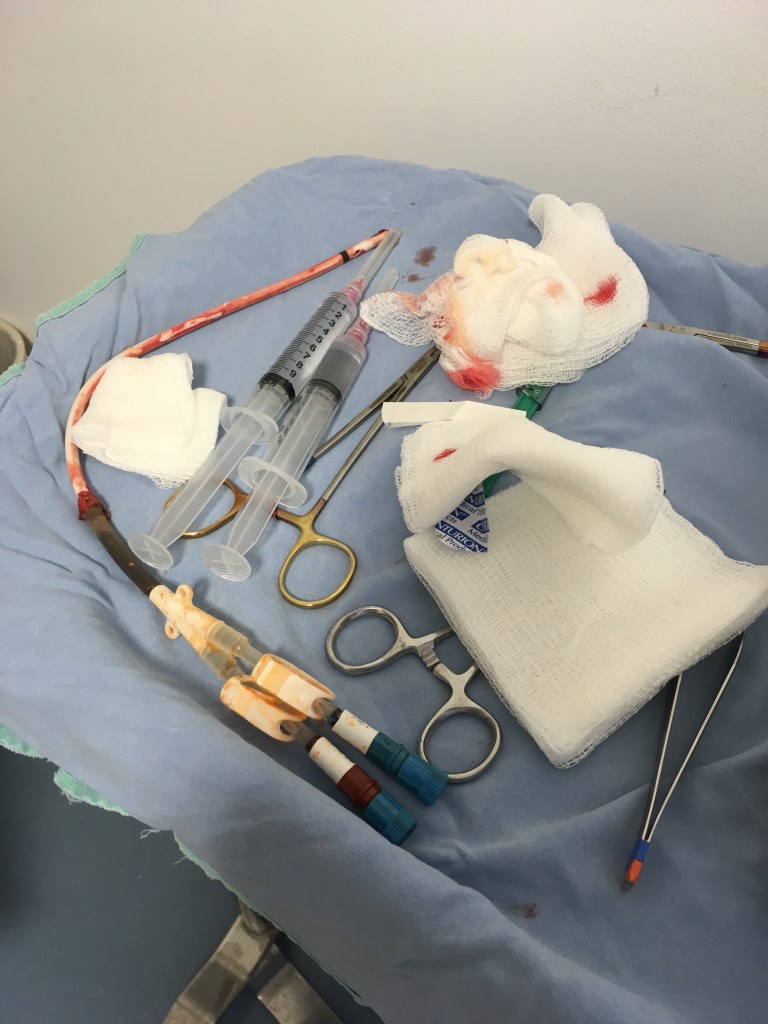
It’s about 2:30 am. I woke up at 2:00 am and haven’t been able to fall back asleep. I’ve only slept about two hours so far. Of course, I can catch up on some sleep during dialysis but usually the fistula keeps me awake, and Tuesday is when the nephrologists do their rounds so someone will wake me up.
The dialysis center changed chairs since I started dialysis there three years ago. I think it was before I left for PD. I don’t remember having any problems with the older chairs. The new ones look the same but are brown instead of green. However, they seem to give me lower back issues. Usually the nurses wants your legs up so you can’t fall forward out of your chair. Sometimes that happens when your blood pressure drops too much and faint. With the legs raised, it puts a lot of pressure on my tail bone area and it becomes very sore in about an hour. I then have to put my legs down and sit up straight to relive the pressure. With PD, at least I get to sleep in my own bed.

At least my dialysis center offers patients pillows and (heated!) blankets. When I was at the other dialysis center across the street for about a month, you had to bring everything yourself. No onsite pillows or blankets offered. I’m going to try to sit on a pillow today. The pillows are really flimsy anyway, and try a rolled up blanket as a headrest to see if that helps. Otherwise I end up walking out after the session like an old(er) man.
==========
Wow, list price of the Champion Series 54 medical recliner is ~$2,500. Why is everything so expensive in the world of medical supplies? My home office chair was only $150 from IKEA and I’ve slept in it before.

I think they should upgrade to a full-body shiatsu massage chair. The Inada one from Japan is $8,000 but it looks much more comfortable. And it reclines.
==========
Update: 7:32 pm
Well, that didn’t work out any better. I tried to sit on the pillow this morning and grabbed an extra blanket as a headrest. The pillow didn’t do anything since it was very flimsy. As soon as the air was squeezed out, it became flat as a bedsheet. The blanket-pillow was better since it provided more support but since I rolled it up to get more height, each time it fell down to the base of the backrest, it was impossible to retrieve and put back under my neck. Initially, this was with both arms free. After they stuck one needle in my fistula so I can’t move it, it was super hard to reposition the pillow and the blanket. I think my butt hurt more than before so I’m not sure what to do. Maybe I need to bring in a nice firm seat cushion to sit on.

:max_bytes(150000):strip_icc():format(webp)/RENAL_DIALYSIS-56a275235f9b58b7d0cac1e2.jpg)