UCHealth Denies Kidney Transplant To Unvaccinated Woman & Donor
AURORA, Colo. (CBS4) – A Colorado woman with stage 5 renal failure was months away from getting a new kidney. Now, she and her donor are looking for another hospital after learning UCHealth’s new policy.
According to UCHealth, the majority of transplant recipients and living donors are now required to be vaccinated against COVID-19. Neither woman has received their shots.
https://denver.cbslocal.com/2021/10/07/uchealth-kidney-transplant-covid-vaccine/
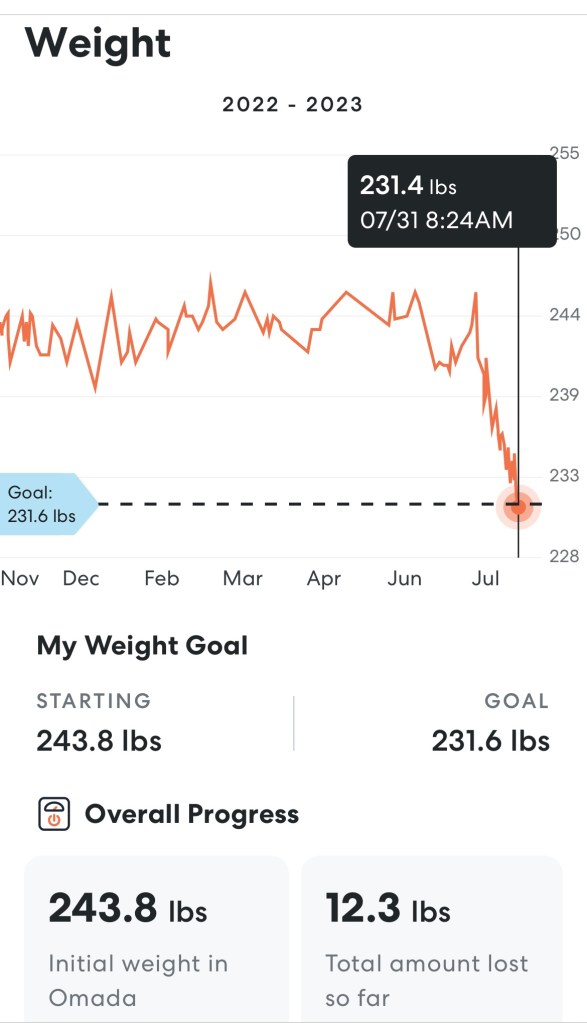
So when my transplant was scheduled in late January, I was not yet eligible for a COVID shot. Unlike the two women in the article, I was super worried about getting COVID in the hospital and losing the kidney after waiting 4+ years. As I posted before, UCLA was basically out of ICU beds, and I had to share recovery with another patient, both of us crammed into a room designed for one bed.
Further down, the article says:
“It’s your choice on what treatment you have. In Leilani’s case, the choice has been taken from her. Her life has now been held hostage because of this mandate,” said Fougner.
Fougner says she hasn’t received the vaccine for religious reasons. Lutali hasn’t gotten the shot because she says there are too many unknowns. Until last week, neither woman thought they needed to be vaccinated for the transplant.
You can tell they are anti-vax idiots by their hyperbole. Really, “held hostage!?” Nobody is forcing them to do anything. They are free to find another transplant center (good luck!) that will do the procedure without requiring vaccinations. Both the reason they give is totally bullshit as well. What religion forbids a mRNA vaccine yet allows for a complex surgical procedure with lots and lots of different drugs. Is she not going to take anti-rejection medication post transplant? Those have more side-effects than any COVID vaccine. The donor is also stupid with the “too many unknowns” crap. There are hundreds of things that can go wrong with both donor and recipient post-transplant. I am pretty sure they had to follow a bunch of appointments and test to get to this point in the process; for sure me and my sister did. Are they going to reject what their doctors and surgeons are telling them at the very last step? Ugh.
Another thought. What if the recipient is willing to get a vaccine? Will the donor say “fuck you” and not go through with the donation if she needs to be vaccinated?
“Here I am, willing to be a direct donor to her. It does not affect any other patient on the transplant list,” said Fougner. “How can I sit here and allow them to murder my friend when I’ve got a perfectly good kidney and can save her life?”
The women haven’t been able to find a hospital in Colorado that will do the transplant while they’re unvaccinated. They’re now looking at other states.
More hyperbole. It is not murder. If the transplant recipient values anti-vax nonsense over her own life, then so be it. My prediction? They will come crawling back to the initial transplant center as they will not fine anyone else to do the procedure.