I was planning to go to cardiac rehab right after dialysis today. Dialysis ended at 1:00 pm and I had a pre-surgery assessment call at 3:00 pm. I thought I could squeeze in a rehab session in between 1:00 pm and 3:00 pm. Instead, the hospital called me at 1:00 pm, just as I was finishing dialysis. The call ended up lasting until 1:45 pm so I went to rehab at around 2:00 pm.
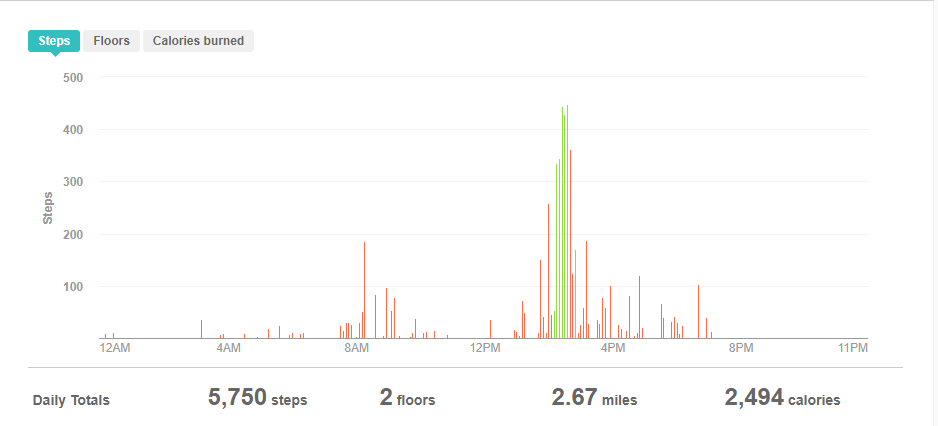
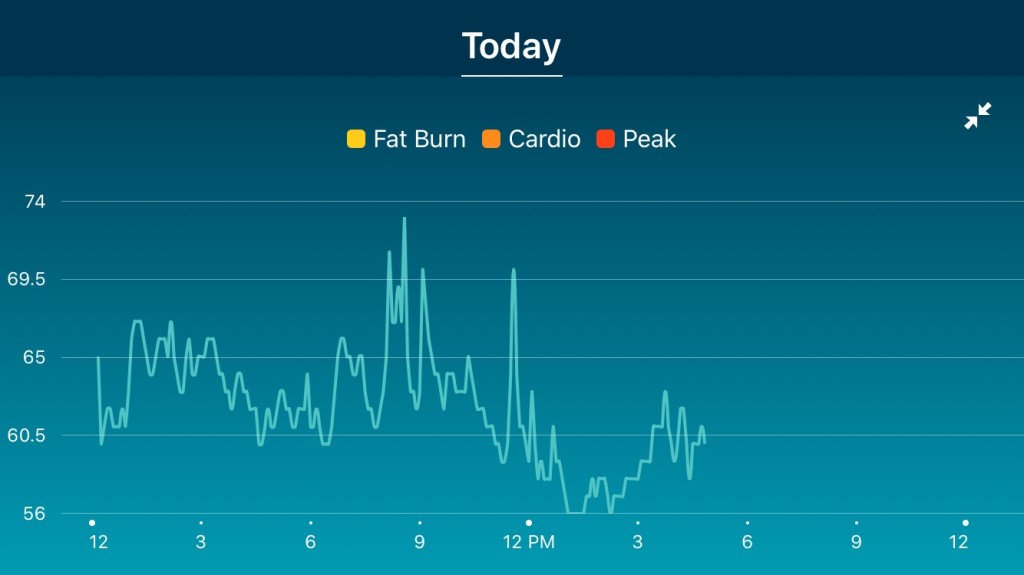
Parking is not free. If you get a validation stamp, then the first hour is free but the next hour is $3.00. Since the rehab is only 30 minutes of cardio plus some arm exercises, you’d think that one could get out in <60 minutes. Nope. You have to check in, then pay, then they take your blood pressure three times: at the beginning, after cardio, and at the end. The two times I attended have taken me about 80 minutes each time so each session is costing me $28 instead of just the $25 insurance co-pay. I still haven’t seen how much the hospital charges my insurance for each workout session.
This is only session #2 so 22 more remaining. I plan on going tomorrow morning at 7:30 am and again this Friday at around the same time. Once I start work, I will need to go MWF at 7:30 am so I can get to work at a decent time.