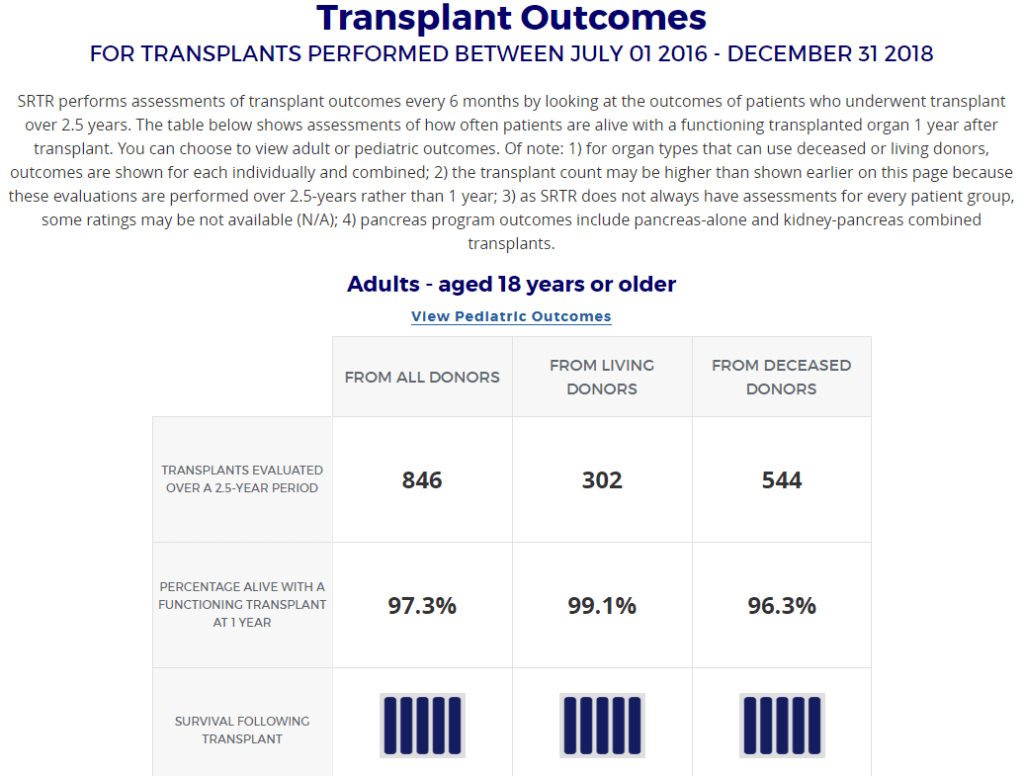
Previously, I wrote a long post trying to analyse wait times for blood type B deceased transplants across several transplant centers. There is another important statistic and that is the survival rate post-transplant. There’s no point getting a kidney transplant quickly then having it fail soon after. Using SRTR data, here are some survival statistics. % alive means percentage alive with a functioning transplant at 1-year. Survival is a five point rating from SRTR.
| Transplant Center | % Alive Living | Survival Living | % Alive Deceased | Survival Deceased |
| UCLA Medical Center | 99.1% | 5 | 96.3% | 5 |
| Cedars-Sinai Medical Center | 100.0% | 5 | 94.9% | 3 |
| St. Joseph Hospital | 100.0% | 4 | 100.0% | 4 |
| Keck Hospital at USC | 100.0% | 4 | 95.3% | 4 |
| UCI Medical Center | 97.0% | 3 | 96.3% | 4 |
| UCSF Medical Center | 99.6% | 5 | 96.9% | 5 |
| UC Davis Medical Center | 98.6% | 4 | 93.5% | 1 |
| Mayo Clinic Hospital | 99.4% | 4 | 94.9% | 4 |
| University of Washington Medical Center | 100.0% | 4 | 98.5% | 5 |
| Methodist Specialty and Transplant Hospital | 98.5% | 4 | 93.1% | 1 |
| Jackson Memorial Hospital | 98.1% | 3 | 93.2% | 3 |
It doesn’t seem like the survival score is correlated with the actual % alive number. Maybe the survival score is more dependent on a longer time scale? From the list above, only UCLA and UCSF scored fives on survival for both living and deceased donors. If I was more worried about transplant outcomes, then the best option is probably to stay listed at UCLA since UCSF seems to have a ridiculously long wait time. Otherwise, Mayo Clinic and UW seem to be good alternatives: large program close by with good outcomes and shorter wait list.