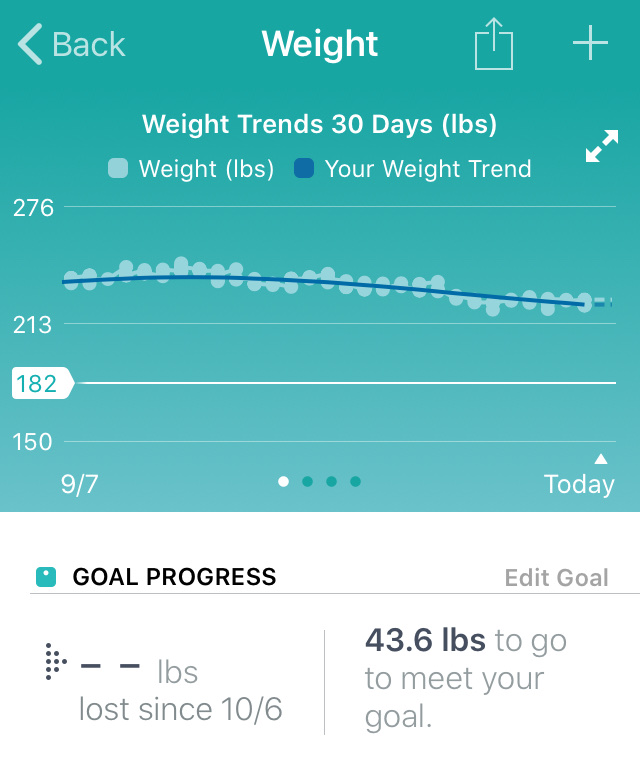
A lot has happened since last Monday. It’s now Monday morning at 4:20am and the past week has been very eventful. I did have a heart attack Sunday night and I ended up needing an emergency heart bypass surgery. The surgeon performed four CABGs or Coronary Artery Bypass Graft on me, replacing arteries in my heart with veins from my leg. This is your classic open heart surgery scenario where they saw through your sternum and crack open your rib cage. I now have about two months of healing to do with no work or driving allowed.
They also did TMR or Transmyocardial Laser Revascularization while inside, drilling little hole in my heart with a laser. Overall it took seven hours for all the procedures and I heard everything went well.
Here is a summary of each day in the hospital so far:
Monday, November 11th
- Went to St. Joseph hospital ER
- Was admitted to hospital for observation with heart in arterial fibrillation
- Troponin levels at 4.5; normal is 0.00 to 0.40
Tuesday, November 12th
- Tropinone levels at 11 indicating heart tissue damage from heart attack
- Emergency angiogram performed and found four badly blocked arteries
- Bypass surgery scheduled for Thursday
Wednesday, November 13th
- Since PD wasn’t working for me anymore, we decided to have another surgery to put in a catheter for hemodialysis; I’ve had one installed before so this was my third dialysis catheter in six months and more holes in my chest
- Catheter in and starting hemodialysis again; a real PITA when you can’t drive anymore
- Threw up when they give me too many blood pressure drugs and my bp dropped to 80/40
- Having major doubts regarding doing surgery, I.e., maybe just fading away would be easier on everyone (more later); brothers from small group visits me in DSU
Thursday, November 14th
- Completely shaved in bed by nurses in prep for open heart surgery; only left armpits and top of head unshaved
- senior pastor from my parent’s Church prays over me in Chinese; read a passage from Isaiah 50, will need to check out later
- Seven hour surgery to do a couple of things to my heart so it’s not broken anymore; beginning of new life
Friday, November 15th
- Wake up at 4am from surgery and breathing tube removed
- Recovering in ICU with blood and fluids draining from chest cavity
- Tried walking and got all dizzy and nauseous; threw up again
Saturday, November 16th
- Moved out of ICU and into cardiac telemetry ward
- Chest tubes removed
- Started eating without throwing up again thought food selection choices are very limited (renal and cardiac)
Sunday, November 17th
- Healing under observation; vitals check every 3 hours so no sleep for extended periods of time
- Sore everywhere, especially when coughing; feels like chest going to split open; also lots of pain in never used back muscles
- Lots of visitors and time to contemplate meaning of this week in God’s Kingdom: why me, where was God in all this, what about grace and healing, what am I going to do with my new life?