I hate this time of recovery. I’m supposed to be resting and getting well, but in reality, I’m sitting around a lot and thinking about how lame my life is and how I got here. More and more I’m regretting the decisions or inaction of my past. Looking back, I can see that I was pretty arrogant, thinking that I was smarter and better than the average person, so I deserved a better life. Ha! Now it’s all regret about how stupid I was.
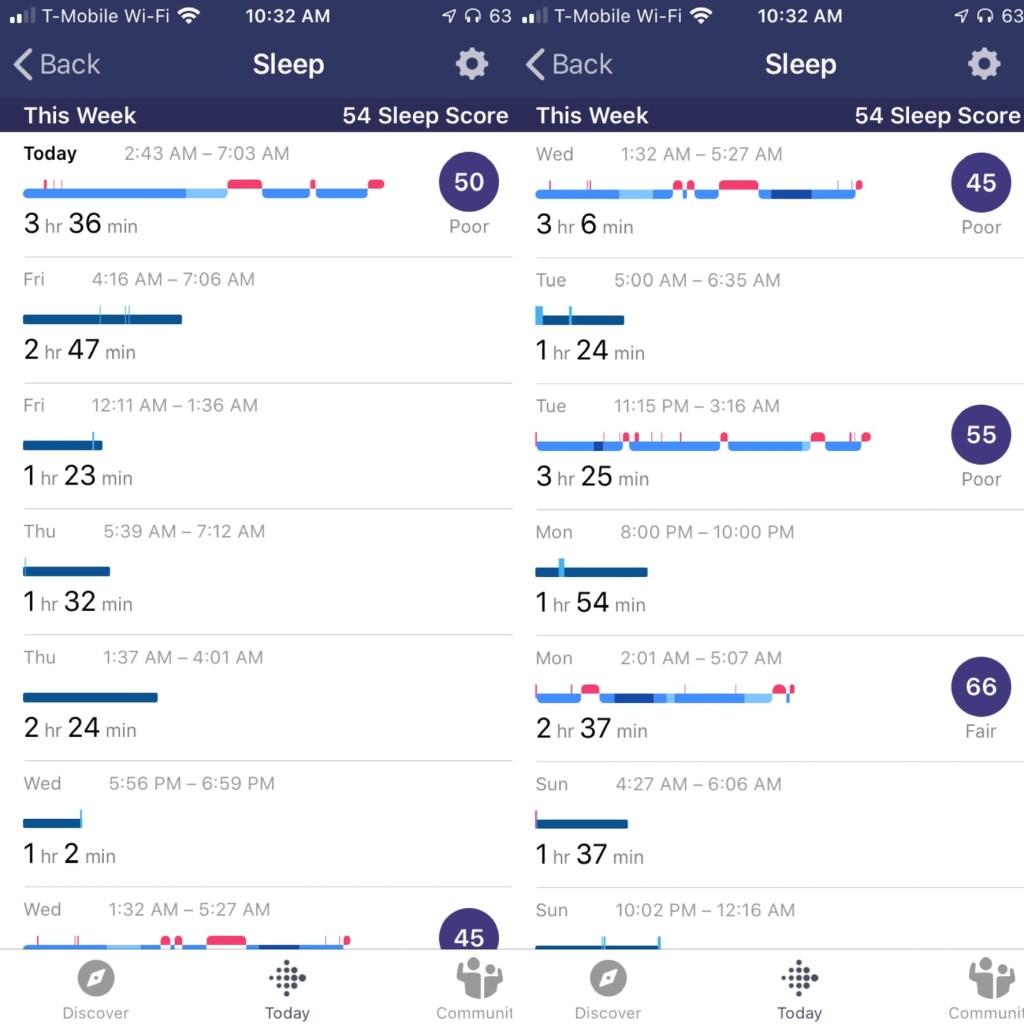
When I got divorced, it was a pretty dark time. I think I was suffering from depression and having the weirdest thoughts. I know after a few years, I believed the divorced was mainly my fault, that I was a poor husband and partner. That was okay but I let my health lapse, thinking anything that happened was deserved punishment. I stopped seeing doctors and also stopped taking my diabetes and hypertension medication. I clearly remember getting a blood glucose reading of 532 on my home meter and not reacting to it. Stupid. I also thought that if I died at 50, then so be it. I’m now 51 and likely almost died several months ago but ended up with bypass surgery instead.
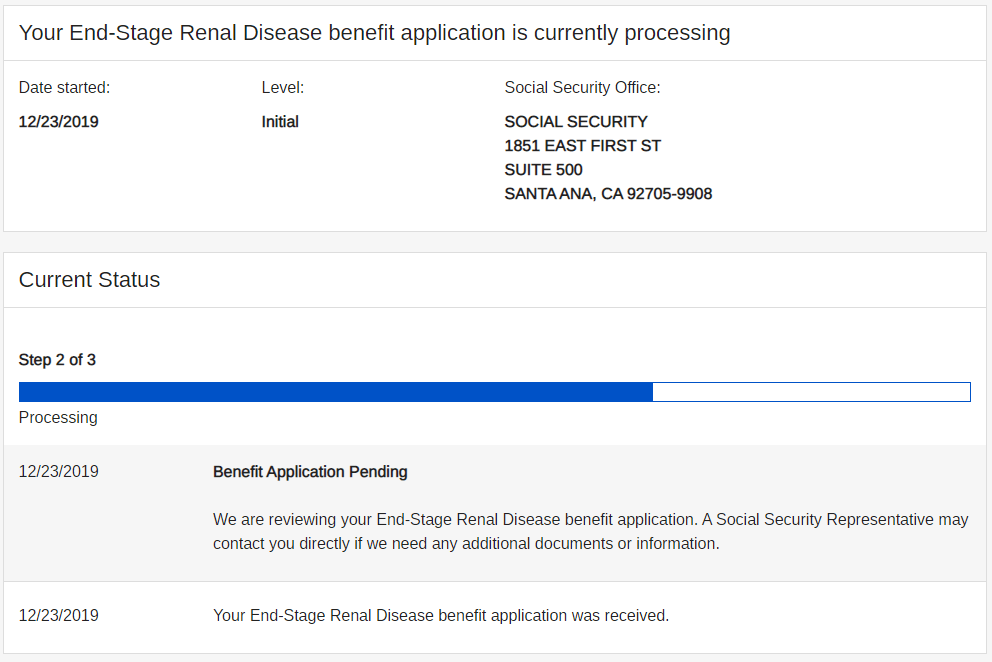
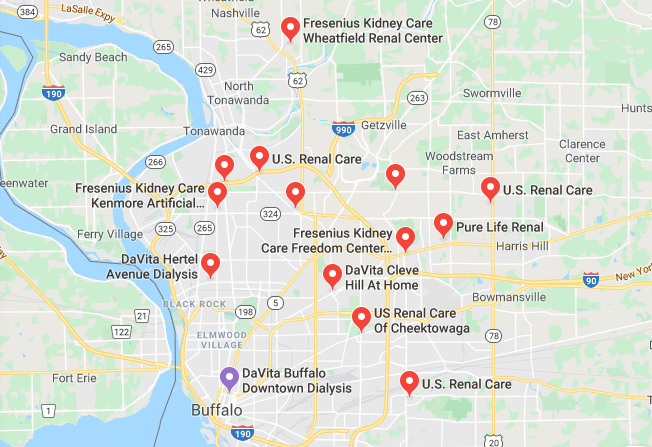
What if? What if my wife didn’t leave me? Would I have taken better of my health? If I wasn’t alone for the past 13 years, would I be more diligent with doctor visits? Would I be suffering from kidney failure now? Of course the answer is yes, yes, and most likely no. But would I be in a better place? Is still being married and not needing dialysis better then my life now? Sigh…
The problem is having these thoughts 24/7 is not helping my current circumstances. I know I screwed up, causing my kidney failure and recent bypass surgery. However, I can’t seem to stop thinking and regretting the past and I can sometimes feel the feeling of depression coming back again.
I just started a short 5-day devotional on YouVersion called It’s Not Supposed To Be This Way. The response question asks “How is your view of God impacted when reality doesn’t align with the way you’d like things to be?” I guess that’s the important question. I just want to be “normal” now. How does dwelling in the past affecting me? Not just with God, but with my parents, sister, friends, church people, coworkers? I don’t want to be that guy, always grumpy and depressed but it feels inevitable.