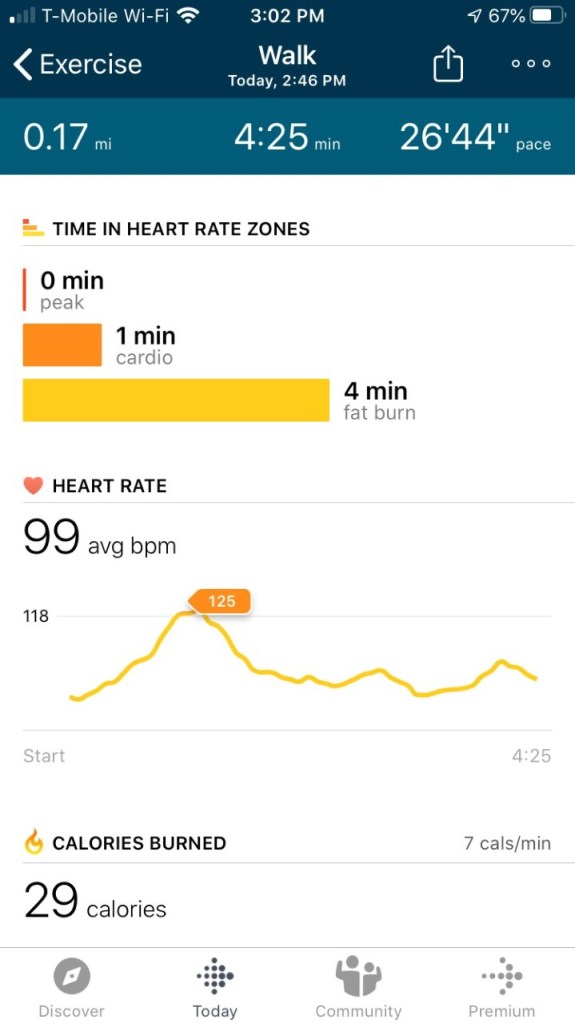
I went to my sister’s house around lunchtime today and walked their dog. The Fitbit tracker failed again halfway but I only walked 0.72 miles at a pace of ~30′. It was harder with the dog since she is easily distracted and does not walk in a straight line. She also pooped twice.
I’m back home and it’s only 4:00 pm. The temperature outside is ~65 degrees and there is still light out so I think I’ll walk some more. It’s got to get easier at some point.
==========
OK, since this post was still up on my computer, I’ll just add to it. I walked 0.72 miles at a pace of 23’38”. It felt much colder than 65 degrees since the sun was going down. I also noticed an intermittent pain in my right ankle. I hope it’s not from walking; I didn’t even walk that much.
During both walks, I felt tired again. Near the end of the walk with the dog earlier, there is a very slight uphill, barely noticeable. However, I started breathing hard like I was climbing Half Dome or something. It was a bit embarrassing and worrisome. How am I going to get through Cardiac Rehab if my heart is still so weak after seven weeks?